Should doctors prescribe blood thinners to covid patients?
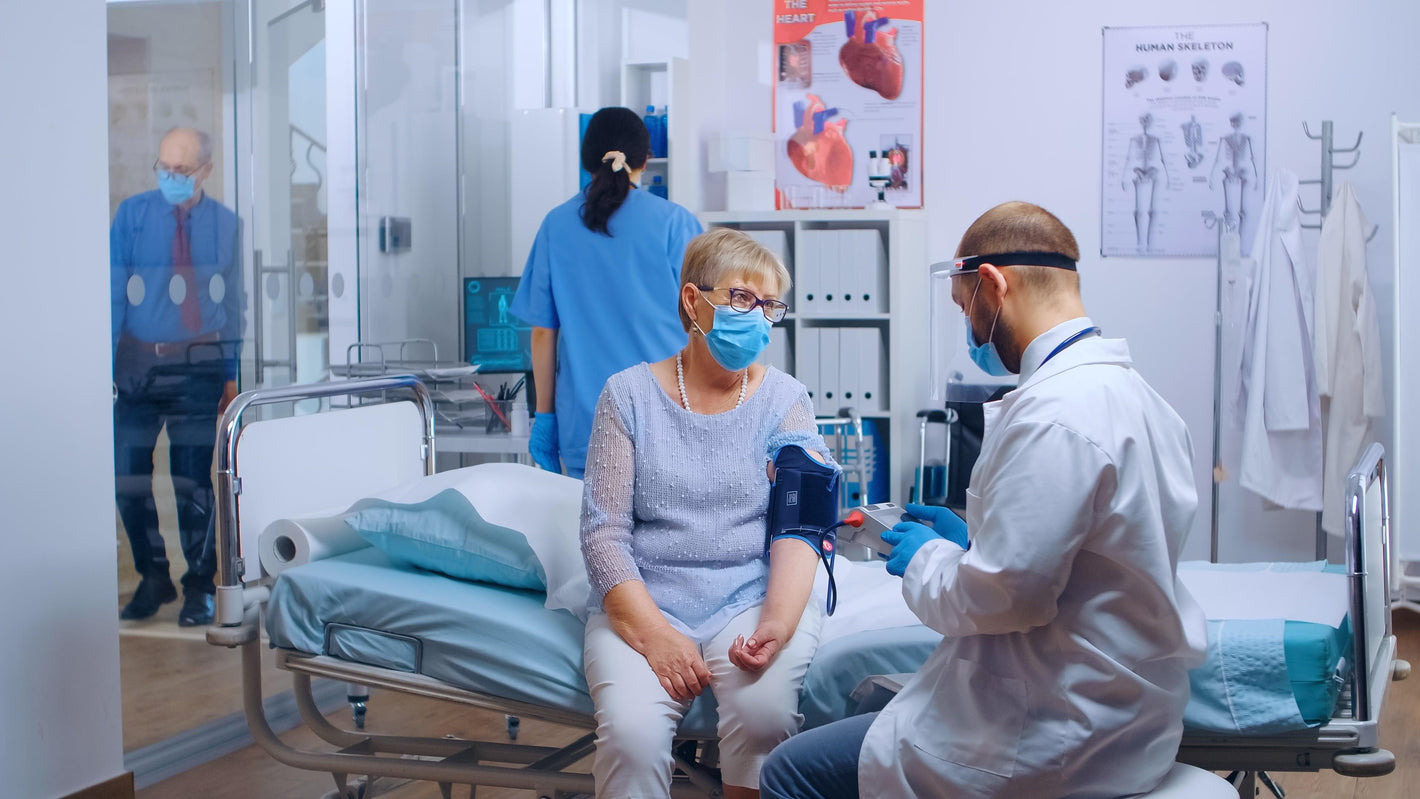


Blood thinners and anticoagulants are medicines used to prevent blood clots in the blood vessels. They assist in the smooth flow of blood in veins and arteries. They are part of standard treatments prescribed for patients at higher risk of clot formation due to heart diseases, diabetes, and blood problems. Patients suffering from COVID are at higher risk of clot formation, especially during recovery. They can develop dangerous clots in their blood vessels that can lead to stroke, heart attack, organ failure, and other complications.
So, the answer to the question mentioned above in the title is a "YES ."The use of blood thinners helps mitigate complications in COVID patients and is recommended by multiple international funding organisations and UK medical research council.
Still, there is a need to consider many factors and precautions. Before diving deep into the topic, let us know more about blood thinners.
If you are more interested in an overview of COVID-19, then read our comprehensive guide written by Dr. Williams, which includes symptoms, causes and testing for COVID-19.
There are two types of blood thinning agents called “Anticoagulants” and “anti-platelets." Anticoagulants prevent blood clotting and keep the blood cells from joining and turning into lumps. They are essential to the hospital's blood collection bags and laboratory sample tubes. The most commonly used anticoagulants are Heparin, Ethylene diamine tetra acetic acid (EDTA), dalteparin, fondaparinux, enoxaparin, rivaroxaban, etc... They are strong anti-clotting factors and compete with vitamin K, which is required to produce special proteins called clotting factors that activate fibrin (A fibrous protein that joins the blood cells to form clots).
The second type of blood thinners are called anti-platelet agents. Platelets are small cell-like bodies present in the cellular portion of blood that unction in clotting and prevent the bleeding from blood vessel haemorrhages. Anti-platelet blood thinner prevents the platelets from joining together and thus prevents blood clotting. The most common Anti-platelet blood thinner is Aspirin. Others include Dipyridamole, Prasugrel, cilostazol, and Tirofiban etc...
Here, it is pertinent to mention that most of the blood thinners routinely administered don't make the blood thin in real, but they prevent it from clotting. Also, they don't break existing clots but avoid new ones.
According to health research published in 2021, the Coronavirus (SARS-COV2) binds to the receptors (ACE-II receptors) on the surface of cells of the wall of blood vessels. This binding and infection cause injury in the blood vessels. This injury causes an accumulation of platelets at the site, which prevents further injury but leads to the formation of blood clots that can be dangerous. On the other hand, vascular damage is also caused by the inflammatory substance produced due to infection, which indirectly causes the production of blood clots. Moreover, reports suggest the presence of autoimmune antibodies that can cause vascular damage leading to the formation of blood clots
Blood clots, when formed, can be fatal if they block blood vessels in an organ. A blood clot can cause the blockage of blood supply to an organ or a part of the organ, leading to blocking the oxygen and food supply to that tissue starving the cells to death. A single clot in an artery supplying a vital organ completely or partially blocking the blood flow to that vital organ can lead to organ failure and death. This is one of the major causes of death in COVID patients after lung damage.
According to the treatment guideline issued by the National Institute of Health for hospitalised COVID patients, anti-thrombotic therapy is vital. The guidelines suggest that the patient already on full-dose blood thinners due to some underlying disease should continue taking them during hospitalisation. Also, the patient not previously on blood thinners should be kept on blood thinners until there are signs of bleeding. So, blood thinners are vital to saving the lives of severely affected COVID patients.
Although the blood thinning agents provide a lot of support in improving clot formation universally, the mechanisms of clot formation and the body's capability to respond to blood thinners vary from person to person. Therefore, the dose, time of blood thinner intervention during the course of the disease, and length of treatment period are different for each patient. According to a study, the full dose, i.e., recommended therapeutic dose of heparin anticoagulant, is not very effective in critically ill patients and doesn't improve their chance of survival. On the other hand, the full dose of blood thinners helps significantly improve non-critically ill (moderately ill) patients and increases their chance of survival. Many clinical trials on the topic are undergoing.
Here the question arises, "What is the difference between critically and moderately ill patients?" Critically ill patients are those who need organ support, i.e., ventilators, etc..., and are intensively cared for at the hospital, while moderately ill patients don't require organ support. Also, The World Health Organization recommends the use of low doses of anticoagulants for the prophylactic after discharge from the hospital as a follow-up.
Although blood thinners are helpful and keeping blood a bit thin may support in improving fatigue and other disease complications, blood thinners should never be used without the prescription and advice of a doctor. When taken for longer, they can cause severe blood leakage problems and impairment of the normal blood clotting process. Prolonged use of blood thinners may cause
If you are advised of blood thinners by your doctor and face any of the above-mentioned signs, you should immediately contact your physician to adjust the dose and evaluate the need for further use of anticoagulants. Also, you should avoid games and sports involving a higher risk of cuts and bruises i.e., blood with anticoagulants takes much longer to clot.
The covid 19 virus has affected multiple organs. Blood thinning agents provide support in the prevention of blood clots in COVID patients, improve their chance of survival, and help in the mitigation of COVID complications. But, the type of blood thinner, length of treatment, dose and dosage, and time of intervention should be decided by certified experts. Moreover, the monitoring of COVID patients prescribed blood thinners is necessary.
If you are concerned about your cardiovascular health, Welzo offers several blood tests that can help you understand your health. See our Heart Health Blood Test here.
We also have a Covid-19 Antibody Blood Test that can help you monitor your covid antibodies. See our test here.










Plus get the inside scoop on our latest content and updates in our monthly newsletter.