
 Instagram
Instagram
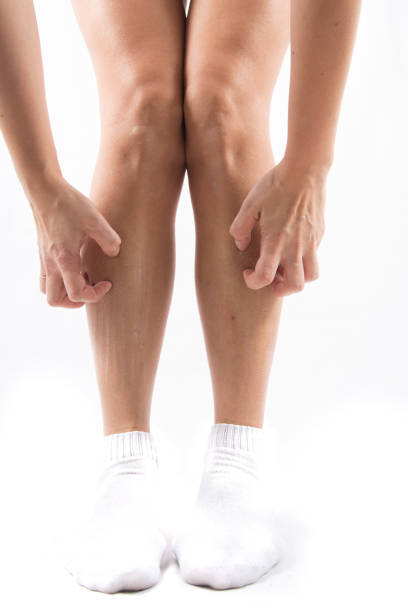
What Causes Itchy Legs Below the Knee?
Related products
The frequent sense of itchiness below the knee, an issue affecting a vast population worldwide, is often associated with considerable distress and annoyance. This widespread affliction, commonly known as 'Pruritus,' typically targets lower limbs. A multitude of conditions might induce this location-specific itching, highlighting its diagnostic complexities and illustrating why understanding probable causative factors is pivotal.

Being a common symptom that instigates more than 7 million outpatient visits every year across the United States alone, pruritus holds significant attention within healthcare communities. The genesis behind such itchy experiences beneath the knees spans a broad spectrum - starting from skin-related complications like dryness (xerosis) or unique rashes to circulatory disorders exemplified by Peripheral Artery Disease (PAD), neurological challenges, namely neuropathy, even systemic illnesses inclusive kidney failure stand implicated within expansive array potential contributors.
Therefore, recognizing critical reasons contributing to itchy lower limbs forms an essential part of the path towards effective remedy identification, thereby enhancing overall mental well-being amongst affected people.
Common Causes
Dry Skin(Xerosis)

Dry skin, medically known as xerosis, is often the most common cause of itchy legs below the knee. This condition presents with flaky or peeling skin, which appears dull and lacks elasticity. In severe cases, cracks on the surface might be visible, leading to a rough texture.
Several factors contribute to dryness, including cold weather conditions where humidity levels are low, causing moisture loss from one's epidermis; overuse of harsh soaps that strip away natural oils protecting our skin; and prolonged immersion in water, particularly hot baths/showers, which have a similar dehydrating effect. Ageing naturally decreases oil production, making older individuals more susceptible to developing xerosis.
Managed effectively through simple preventative actions—such as avoiding excessively long showers/baths, especially using steaming-hot water, and opting for mild soap variants rather than heavily perfumed/scented ones or those with high alcohol content—these measures assist in preserving integral hydration within one's dermal layers, thereby warding off undue dryness.
Treatments focus on rehydration and restoration of lost moisture into the affected area via the application of topical moisturisers/lotions-rich emollients like glycerin & ceramides plus humectants (substances promoting retention). Over-the-counter creams containing lactic acid or urea assist by gently exfoliating dead cells, relieving itching and improving overall appearance. Creams and lotions for dry skin are available at Welzo, including Nivea Lotion and Bio-Oil Dry Skin Gel.
For persistent issues despite self-care regimen adaptations, consulting healthcare providers becomes imperative since prescription medications incorporating intensive hydrating ingredients become necessary, along with ruling out any hidden underlying systemic reasons behind pervasively parched skin manifestation.
Contact Dermatitis

Contact Dermatitis, a common cause of itching sensations below the knee, is an inflammation-triggering reaction incited by direct exposure to specific substances. This condition chiefly encompasses two categories: irritant contact dermatitis and allergic contact dermatitis.
Irritant Contact Dermatitis constitutes the more frequent variant - manifesting after leg skin interacts repetitively or intensively with harmful chemicals like soap/detergents, bleach or even mild irritants such as water when overexposed.
On the other hand, Allergic Contact Dermatitis arises from sensitivity to specific allergens; common examples encompass nickel (found in jewellery), rubber boots/latex gloves, and poison ivy/oak plants—all potent triggers despite brief encounters only.
Diagnosis typically involves a comprehensive medical history review alongside a physical examination. For definitive confirmation - particularly useful when ruling out lookalike conditions such as eczema- Patch Testing becomes necessary, whereby suspected allergen pieces are applied onto the patient's back for around 48 hours, observing resultant reactions.
For treatment methods, patients have many viable options at their disposal depending primarily on severity extent coupled by an involved causative agent, which forms their tits basis. Topical corticosteroids seem highly effective against inflammation symptom reduction, while oral antihistamines cater towards the alleviation of itching sensations. Both are recommended widely amongst practitioners' circles.
Education serves a pivotal role akin to regularly emphasising the importance of avoidance protocol adherence once the offending substance is identified. It relies not alone on medicinal therapies but proactive prevention strategies to help prevent future recurrence episodes, thus ensuring a healthier, happier life ahead.
Eczema

Eczema, scientifically termed Atopic Dermatitis, has risen to prominence among dermatologists and health practitioners due to its high prevalence. Known for causing inflammation of the skin characterised by dryness and itchiness, this condition often appears in patches on various parts of the body, including lower extremities such as legs below the knees.
Different types include Dyshidrotic Eczema, manifesting as small fluid-filled blisters that flare up during specific seasons or stressful periods; Nummular Eczema, recognizable as coin-shaped spots that are intensely itchy and often occur post-skin injury; and Stasis Dermatitis, triggered primarily among individuals suffering from venous insufficiency, leading to itchiness concentrated around ankles and calves.
Presentations distinctive to lower limbs encompass persistent itching, often accompanied by red rashes, which might progress into bumps oozing liquid upon scratching them excessively, eventually followed by crusting over or scaling.
Management strategies include regular moisturization utilising hypoallergenic creams, which form the first-line defence against preventing the onset and thereby circumventing the worsening of symptoms once they have appeared.
Diabetes

Diabetes often heralds a range of associated complications—among these, itchy skin emerges as an uncomfortable yet prevalent symptom. High blood sugar levels disrupt normal body functions and instigate myriad problems; pruritus or itchiness stands among these consequential issues.
When investigating the science behind diabetes-induced itching, medical experts highlight two primary factors: dry skin and poor circulation. Internal hydration levels regulate both processes and are effectively moisturised via natural oils produced by sweat glands. Elevated glucose in the bloodstream disrupts both processes, giving way to excessive drying and causing significant itchiness.
Shifting focus specifically below knees highlights directive issues related to decreased vascular supply – essentially constituting peripheral areas of our body owing to their distance from the heart sidelined during circulatory resource allocation, especially when compromised, such as found within diabetic situations, which favours the formation of Peripheral Artery Disease (PAD). Chronically diminished blood flow causes local tissues to starve, leading to intense itching sensations typically experienced below the knee.
Poor Circulation
One common cause of itchy legs below the knee is poor circulation, a condition characterised by inadequate blood flow to various body parts. Lower extremities like legs are often affected due to their distance from the heart and gravity's effects.
Inadequate circulation predominantly stems from conditions such as peripheral artery disease (PAD), wherein narrowed arteries reduce blood supply notably into your limbs. PAD patients frequently report experiences with pruritus - commonly attributable to insufficient oxygen delivery across bodily tissues.
Impaired circulatory functionality exacerbates dry skin or xerosis, which in turn instigates itching tendencies in the lower limbs. Furthermore, diminished nutrient transport, consequent upon decreased perfusion, might contribute to neuronal health degradation, leading, on occasion, to neuropathy, which is characteristically associated with sensations similar to leg pricking mentioned hereinbefore.
Itching typically remains accompanied by changes in skin colouration due to reduced nourishment status or feelings akin to tingling/numbness resulting from nervous function impairments, a secondarily reduced oxygen availability scenario explained previously.
Treatments target underlying disease processes besides symptomatic relief, ensuring problems don't re-emerge soon after. For instance, doctors advise incorporating regular exercise and healthier diet choices to reverse arterial narrowing seen amongst PAD sufferers, while topical creams/moisturisers suggest combating dermal drying issues. Additionally, neuropathic pain management options extend symptom mitigation facilities for ones grappling with nerve-induced troubles alongside treating causative systemic ailments if involved therein patient context-specific case analysis basis.
Insect Bite

Primary triggers for pruritus, commonly known as itchy legs below the knee, frequently include insect bites. Usual suspects encompass mosquitoes, ticks, fleas and chiggers – each infamous for provoking discomfort through their irritating nibbles. Identifying the insects in question is critical to charting a suitable path towards managing itching induced by these tiny troublemakers. Mosquitoes leave small red swollen spots that start tingling soon after bite incidence; on contrast, tick bites display diverse symptoms, possibly showing rashes accompanied by intense itch at the biting site, whereas flea nips typically form clusters appearing as small reddish bumps encircled within similar coloured halos.
Prevention remains key to preventing fungal infections, which frequently occur secondary to improper scratching post-bite. It is advised to utilise repellents containing DEET (N, N-Diethyl-meta-toluamide) or wear long pants during outdoor activities, especially at dusk, when many insects are most active, thereby minimising exposure risk substantially.
Upon experiencing the condition, many readily available antihistamines have demonstrated their effectiveness in diminishing inflammation. Similarly, topical ointments enriched with hydrocortisone are recognized for easing discomfort and lessening levels of skin surface swelling.
Skin Infections
Persistent itching below the knee often finds its roots in various skin infections. Two dominant types prevalent among patients are fungal and bacterial infections.
Contrary to popular belief, fungi aren't only found on stale bread or rotten fruits; they're virtually everywhere - air, soil, and water. When conditions favour them, like warm, moist environments such as sweaty socks or shoes, these microbes might colonise human skin, triggering an infection known medically as 'Tinea'. Ringworm is a classic condition that affects the legs, specifically in athletes who tend to retain sweat for prolonged durations post-exercise.
Distinct indicators include red-scaled patches bearing clear borders and intense itch localised mainly around calves and the shin area. Sometimes, there's accompanying foot involvement (Athlete's Foot), too.
Bacteria generally inhabit our body surface without causing harm until something disrupts their homeostasis, propelling an invasion into deeper layers of your epidermis and leading to cellulitis – typical symptoms encompass swelling besides erythema coupled with extreme tenderness but invariably presenting persistent itches restricted beneath knees predominantly around calf muscles alongside fever occasionally.
Treatment strategies largely hinge upon accurate diagnosis, furthered by selecting appropriate antimicrobial therapy, usually lasting 1-2 weeks, depending upon the severity involved and patient compliance with prescribed drugs. Antifungals for tinea and antibacterials against cellulitis must be taken exactly per physicians' advice, ensuring timely follow-ups.
Failure to treat underlying causes paves the way for recurrent episodes, hence the need to stress the importance of preventive measures, from basic hygiene practices, including avoiding sharing personal items, to drying feet well before wearing footwear.
Other Causes
Nerve Disorders
Some less common but noteworthy causes of itchy legs below the knee are nerve disorders. Neuropathy, a condition characterised by damaged nerves mostly from the peripheral nervous system (not in the brain or spinal cord), is one ailment that brings along irritation and itching as symptoms despite no visible skin changes explaining those sensations, particularly among diabetics.
Neuropathy might trigger severe itch, specifically over feet extending up to the lower leg, typically described as an "ants crawling up down" feeling. Patients often report onset during the night, adversely affecting their quality of sleep and, thus, life overall.
Non-pharmacological approaches involving acupuncture or transcutaneous electrical nerve stimulation have shown promising results. At the same time, drug treatments often constitute capsaicin cream application for localised relief, supplementing systemic therapy comprising anticonvulsant drugs like pregabalin, which are managed under careful medical supervision and become essential here.
Systemic Conditions
Systemic illnesses, namely liver diseases & kidney malfunctions, paint another picture behind pruritus pathogenesis. Under conditions when these organs fail to function adequately - toxins accumulate within the body, creating an internal environment that irritates nerves, thereby causing persistent itches, usually observed more in extremities, including regions beneath knees, amongst others.
The diagnostic approach begins with taking a detailed patient history followed by comprehensive examinations alongside blood tests confirming organ damage, if any, based upon which treatment gets planned out, mainly targeting disease control plus symptom relief incorporating a combination of medications accompanied by non-drug methods customised per individual case scenario needs to be aimed towards better health outcomes achieved through rigorous follow-ups.
Medications
Certain medicines-another significant contributor towards itchy ailments are scarcely mentioned in discussions around the subject matter yet hold considerable relevance to the problem-posing hand because myriad drugs display 'itch' as a potential side effect given how they interact on a molecular level interfering with normal biochemistry underlying skin's barrier function giving rise incessant scratching episodes seen post consumption; examples include certain antibiotics opiates cholesterol-lowering agents etcetera among plenty others cause mysterious tingling without rash people find hard describe finding solace once offending agent identified quit subsequently.
Identifying such a link, however, isn't straightforward and demands professional insight to elucidate the connection between drug intake and subsequent symptom development. The strategy then becomes either replacing those with alternatives, if available, or managing side effects using antipruritics until course completion is conceived under physicians' close watch, ensuring patient compliance towards the same, thereby safeguarding against unnecessary discomfort stemming from it.
When To See Your Doctor
Experiencing itchy legs below the knee might not always ring alarm bells, yet certain conditions necessitate medical consultation. When itching turns persistent or worsens over time, undeterred by home remedies, if it interferes with daily activities, especially sleep, an appointment must surely be made for evaluation.
In situations where itching accompanies other alarming symptoms like unusual weight loss, systemic complaints such as fever and fatigue, or visual proof of infection, marked redness alongside warmth felt around skin patches carrying severe pain upon touch are tangible indications justifying urgent attention from a healthcare professional seeking expert help right away.
Moreover, if pruritus occurs post-new medication initiation- making correlation becomes crucial, so immediate consultation is advocated to review drug profiles, possibly tailoring subsequent treatment plans based on individual cases.
Last but most importantly, considering increasing incidence rates of diseases globally, particularly diabetes & cancer, both being known causative contributors towards neuropathy thus, leg itch— any tingling sensation without obvious reasons needs checking out to rule potential links given far-reaching consequences involved failing timely detection wherein importance regular health check-ups cannot stress enough.
Home Remedies To Alleviate Itchy Legs Below The Knee
- Moisturising Regularly: Adequate moisturisers should be used, especially post-shower, when skin pores remain open optimally absorbing applied products. This ensures the retention of natural oils, preventing dryness and alleviating itchiness.
- Using Mild Soaps and Detergents: Gentle cleansers without heavy fragrances or dyes maintain pH balance, preserving the skin's essential protective barrier function. They also minimise contact irritants, thus dramatically reducing the chances of lower leg itching.
- Wearing Breathable Fabrics: Natural materials like cotton allow air circulation, avoiding excessive sweat accumulation. They also provide a cool, soothing effect, lessening irritation and, hence, effectively keeping itch away.
Prevention Tips
- Maintaining Hydration Levels: Adequate water intake supports optimal body functioning, including healthy skin. This indirectly helps minimise pruritus episodes, acting as a simple yet effective prevention strategy.
- Avoiding Known Allergens and Irritants: If certain substances known to cause allergy or irritation are identified, it's best to steer clear of them. This includes personal care items with harsh chemicals and specific food types, among others. Remember, 'prevention is always better than cure' applies perfectly here, too.
- Re-establishing Proper Skin Care Routine: A balanced routine involving gentle cleansing followed by sufficient moisturization & regular exfoliation promotes healthier skin, creating a robust defence mechanism against common causes behind persistent tingles felt around areas below the knees, truly justifying its inclusion in daily life habits list, marking the final tip towards achieving that much-carved relief finally ending scratching saga once for all indeed.
Frequently Asked Questions
What is itchy lower legs a symptom of?
Itchy lower legs might be symptomatic of various conditions, including dermatological issues like dry skin or eczema, circulatory problems such as Peripheral Artery Disease (PAD), nerve disorders notably neuropathy, and systemic diseases, including kidney failure and certain liver ailments.
How do you treat itchy lower legs?
Treating itchy lower legs involves identifying the root cause first, followed by an appropriate medical intervention that often combines medication for symptom relief plus tackling the underlying condition responsible. For instance- antimicrobials are prescribed to manage skin infections, whereas controlling blood sugar levels forms a cornerstone during diabetes-induced itchiness.
How do I get my legs to stop itching?
To stop legs from itching, ensure regular moisturization post-shower when pores are the best absorbent. Further, avoid scratching the area, which aggravates the problem. Hence, applying cool compresses helps soothe inflamed regions efficiently. Both suggest simple yet effective measures to obtain instant relief.
Does itchy legs mean liver problems?
Yes, itching can sometimes hint towards liver diseases because these disorders lead to toxin build-up in the body, causing irritation. Thus, tingling sensations, particularly beneath the knees, among other spots, can be evoked, summarising the complex interrelation between pruritus and hepatic illnesses.
What deficiency causes itchy legs?
Deficiency of certain vitamins, particularly B12 and iron, has been associated with persistent leg itch, given their pivotal roles in maintaining healthy nerves and promoting optimal cell growth; hence, it underscores the importance of a balanced diet, ensuring adequate micro-nutrient intake, preventing prickly nuisances, and enhancing the quality of life overall.
Is itchy legs diabetes?
Yes, diabetes is one potential culprit behind relentless leg tickles, most cases attributable to diabetic peripheral neuropathy, a condition involving damage to the nervous system secondary to long-standing uncontrolled glucose levels, painting a clear portrait between this metabolic disorder's significant role in triggering notorious under-knee-itch episodes certainly validating its place within elaborate list causative factors connected phenomenon at hand reinforcing necessity comprehensive treatment strategies aimed beyond mere symptom management truly addressing core issue involved.


















 Rated Excellent by 26,523+ Reviews
Rated Excellent by 26,523+ Reviews