
 Instagram
Instagram
Thrush: Causes, Signs and Symptoms, Diagnosis, and Treatment

Related products
Thrush is a common yeast (fungal) infection. The causative yeast grows in the throat, mouth and other body parts, causing a variety of lesions in these organs. Young children, particularly toddlers, are most commonly affected, although anyone can experience it. Besides the fungus, various risk factors like diabetes, oral diseases, dry mouth and the side effects of some medications also have a role. The incidence rates for each type of thrush are different. For example, 1.2 million women in the UK suffer from vulvovaginal thrush, as shown by a report published by the University of Manchester. Similarly, 30-45% of adults and 45% of neonates experience oral thrush, according to the National Institute for Health and Care Excellence.
Depending upon the organs involved, it causes irritation, redness, and swelling. Despite being so widespread, it is rarely a cause of death, except the invasive candidiasis, which occasionally causes death. Unlike oral or genital candidiasis, where the lesions are mainly localized, invasive candidiasis spreads to other body organs like eyes, bones, blood, brain and heart, leading to severe complications and death in 19-24% of cases, as noted by a research published in 2005 by Juliette Morgan and his colleagues. The treatment options are using local, oral and systemic antifungals to curb fungal growth, antibiotics to prevent secondary bacterial infections, painkillers, and anti-inflammatory drugs to manage the symptoms.
What is Thrush?
Thrush is a common fungal infection of the mouth, external genitals and other organs. It is caused by various fungus species of the genus Candida and is characterized by patchy white lesions in the mouth and other outer body parts, irritation and swelling. Multiple species of fungus are responsible, and they grow on wet skin or mucus membranes (internal skin) wherever conditions like humidity and moderate temperature are available. A weakened immune system paves the way for establishing fungal infection alongside other risk factors.
What is the other term for thrush?
Various terms for thrush have evolved depending on the organs involved, the types of lesions and the causative factors. The standard terms used in medicine are candidiasis (a general term used for the infections caused by all candida species) and moniliasis or monilia disease (monilia being the other name of candida). Depending upon the causative species of fungus, it could be Candida albicans infection, Candida tropicalis infection, Candida glabrata infection, Candida krisei infection, or Candida parapsilosis infection etc. The names are also derived from the site of infection like oropharyngeal candidiasis (oral thrush), genital candidiasis (yeast infection of the external genitals), diaper rashes due to yeast infections or the invasive candidiasis (the spread of diseases to the various body organs).
How does thrush function?
Thrush develops whenever the body's physical or biological balance is disturbed due to any causes. The disruption of host microflora or the loss or deficiency in immune functions causes the opportunistic fungus to grow excessively. The excessive growth of fungus on the skin and mucus membranes causes the desquamation of the epithelial cells and the accumulation of necrotic tissues, keratin and bacteria, causing the characteristic patchy lesions. The debris accumulates and attaches closely to the skin and mucus membranes to form a pseudomembrane.
Sometimes, the development of membranes causes necrosis, ulceration and oedema in the underlying tissues. The neonates get this infection while passing through the infected vagina (if the mother had genital candidiasis). Once a localized infection is established, the fungus reaches the bloodstream through the mucosal barriers of the gastrointestinal tract or through an infected intravascular catheter to cause more dangerous and invasive candidiasis. Invasive candidiasis is familiar to patients with ascending fungal urinary tract infections.
How long does thrush last?
Depending upon the type and severity of infection, the nature of lesions, the treatment options used, and the nature and status of the immune system, it lasts from a few days to weeks and even months. The uncomplicated and mild cases should resolve within 5-7 days, while complicated and treated patients should resolve within 7-14 days. The recurring and severe infections take much longer and need weeks of regular treatment.
Who is at risk of developing a Thrush?
Practically, anyone can develop thrush irrespective of gender, age and lifestyle. However, the people who are at higher risk are infants (under one month) and toddlers, aged people over 65 years of age, people with compromised or weakened immune systems (like HIV patients, diabetics, cancer and liver patients), people using immunosuppressant drugs like some antibiotics, and corticosteroids, people having or had a history of oral diseases like Sjogren's syndrome and dry mouth syndrome, people using dentures that fit poorly, smokers and people with fungal infections in the past.
What are the different Types of Thrush?
Depending upon the type and nature of the infection, the nature of lesions and causative agents, there are several types of Thrush. Some common types are;
- Oral Thrush: It is a fungal infection of the mucus membrane of mouth and pharynx. The candida species cause it and are therefore called oral candidiasis. It is not a severe issue and resolves rapidly with antifungal drugs.
- Vaginal Thrush: Also known as vulvovaginal candidiasis, it is the fungal infection of the vulva and vagina caused by a fungus called the Candida albicans. It is not a sexually transmitted disease but causes a cottage cheese-like discharge, and is often a cause of pain and discomfort and needs to be treated.
- Esophageal Thrush: Also known as oesophagal candidiasis, it is the oesophagus's fungal infection causing pain while swallowing food and water. More than 20 Candida species are associated, the most common being the Candida albicans.
- Breastfeeding thrush: It is a fungal infection of the breasts and causes pain in the breasts and nipples, particularly after a breastfeeding session. It is caused by different Candida species, causing dry, flaky, reddened or bright pink nipples and areola. It is the leading cause of sore nipples.
- Invasive Thrush: Also known as invasive candidiasis, it is the most dangerous type of candidiasis and happens when the fungus breaks the body barriers to reach the blood circulation causing fungal lesions in multiple organs like eyes, bones, brain etc. It is the most deadly candidiasis, causing prolonged hospitalizations and death in 19-24% of cases.
- Cutaneous Thrush: It is a fungal infection of the skin. All types of skin and body areas can develop it, particularly the warm and moist areas of the groin and armpits. The primary cause of cutaneous thrush is Candida albicans. It causes a crusted, red, rapidly spreading skin infection, abscesses, and white plagues.
1. Oral Thrush
As the name indicates, it is a fungal infection of the oral cavity.
Figure 1: Close-up view of a child with Candida lesions on the tongue.
Oral thrush, or oropharyngeal candidiasis, develops when the yeast grows inside the oral cavity. Various yeast species are responsible; the Candida albicans are the most important. Yeasts are among the ordinary residents of the oral cavity, and a complex set of interactions with other microbes keep its population in check. Oral thrush develops whenever the growth of yeast becomes out of control due to the use of immunosuppressant drugs, immunosuppressive diseases, radiation therapy and other causes. It causes yellowing to whitish spots or lesions on the roof of the mouth, gums, lips, tongue and inner cheeks.
Sometimes, the oral thrush progresses to the oesophagus and becomes oesophageal thrush. Toddlers and infants are most susceptible to it. Symptoms are often not noticeable in the initial days. However, severe infections cause the symptoms. For the treatment, home remedies and prescription drugs are used.
Home remedies: Some lifestyle changes, home remedies and maintaining good oral hygiene promises good results. The sound practices are regularly brushing the teeth with a good quality and soft brush, regularly replacing the brush, regularly cleaning and disinfection of oral dentures if used, avoiding mouthwashes and mouth sprays unless recommended by the doctor, regularly rinsing the mouth with saltwater, solution of baking soda, solution of lemon juice and apple cider vinegar etc. The use of probiotics like yoghurt is also very helpful in restoring the balance of oral microflora.
Antifungal medications: Antifungal drugs are prescribed, like clotrimazole, fluconazole, itraconazole, and amphoteric B. Nystatin, another oral antifungal medication, is available as an antifungal mouthwash. In contrast, the others are available as oral preparations like lozenges. Amphotericin B is used in severe cases of thrush.
With rigorous care and early treatment, it resolves within 7-14 days. However, it takes longer if left untreated or is complicated by other oral infections. Many times, it returns, particularly in infants. In such cases, the patients need to consult the doctor.
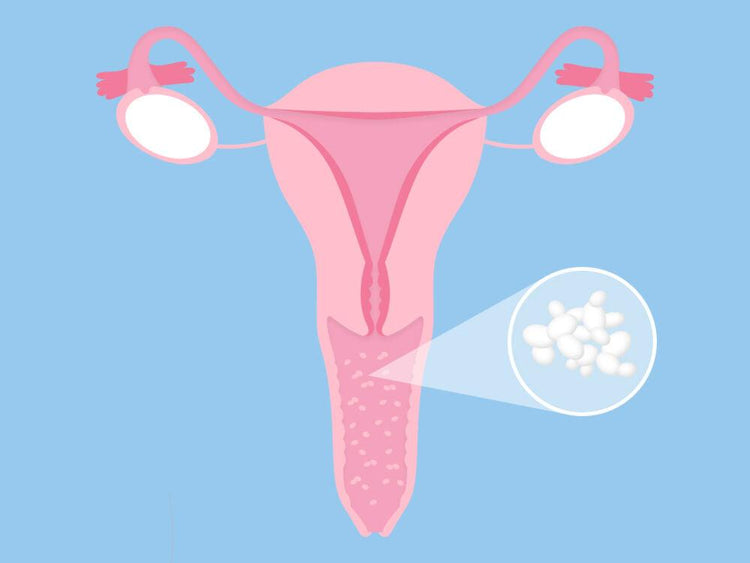
2. Vaginal Thrush
The vaginal fungus infection caused by the imbalance of vaginal microflora leads to excessive fungus growth.
Figure 2: Vaginal fungal infection causes itching and burning sensation.
Like the oral thrush, it also results from the imbalance of normal microflora of the reproductive tract, as it typically has yeast and bacteria. Any factor that disturbs this balance and causes the overgrowth of yeast causes vaginal thrush. It is widespread, and 75% of women experience it at any point in their lives, and 40-45% of women experience more than 1 episode. Various yeast species have a role, but the most important is the Candida albicans. Fungus needs an airless, warm place to grow; the vagina is thus a favourite place to grow.
This fungus is an opportunistic pathogen, which means it is the normal inhabitant of the reproductive tract and causes infections whenever there is an opportunity like a woman is using some immunosuppressant drugs, taking prolonged antibiotic therapy (disrupts the average balance of microflora), is pregnant, receiving hormonal treatments, have severe and unmanaged diabetes, undergoing radiotherapy or chemotherapy or have immunosuppressive diseases like AIDS/HIV.
The vaginal thrush is treated using OTC and prescription drugs. OTC vaginal treatments like antifungal vaginal creams, oral tablets and suppositories containing tioconazole, miconazole, butoconazole and clotrimazole promise some benefits. However, the use should be avoided if a woman is unsure if the symptoms are due to thrush or something else. OTC drugs are risky, and some preparations cause issues like leakage etc. So, the best option is to go to the healthcare provider for diagnosis and treatment.
The doctors prescribe antifungal drugs to treat vaginal thrush, depending upon the patient's condition and the severity and type of infection. These antifungal drugs curb the growth of the yeast and are often used in combination with probiotics to help restore the balance of microflora. Some commonly used antifungal drugs are fluconazole, miconazole, clotrimazole, econazole, fenticonazole and terconazole. They are available as oral tablets, topical creams and gels or suppositories, which are applied directly into the vagina. After a thorough review of the clinical picture, the doctor decides the mode and duration of treatment. A typical treatment is to combine an intravaginal drug with oral medication like fluconazole.
The duration of the disease depends upon the severity. Most mild and uncomplicated cases, even if untreated, resolve within a few days. The treatments often hasten recovery, and severe cases take weeks to recover. With proper care and treatment, it heals within 1-2 weeks. If no improvement is noted after two weeks of regular treatment, the patient must consult the doctor.
3. Esophageal Thrush
Also known as the oesophageal candidiasis, it is a fungal infection of the oesophagus (food pipe). According to NIH, it is a comparatively rare common type experienced by 0.32-5.2% of the general population.
Figure 3: Oesophaeal thrush, an extension of the oral thrush, causes severe pain and irritation in the throat and chest.
The oesophagus connects the mouth with the stomach and often catches infections from the mouth. Many yeast species are responsible, but the most important is the Candida albicans, the others being the Candida Krusei, Candida glabrata, Candida tropicalis and, in rare cases, some other fungal species like Histoplasma or Aspergillus. These are the normal inhabitant of the oral cavity and cause infections whenever the opportunities arise, like weak immunity, immunosuppressant drugs, prolonged use of antibiotics that disrupt normal microflora, and diseases like cancer, diabetes, and HIV/ AIDS.
Some lifestyle risk factors also increase the susceptibility to oesophageal thrushes, like smoking, use of drugs, poor oral hygiene, and medications causing dry mouth as a side effect, and using contaminated dentures. It also develops in people with good immunity that has undergone surgical procedures of the oesophagus.
Like other fungal infections, it is treated through home remedies and prescription drugs. The home remedies work well for oral candidiasis. Still, oesophageal thrush is a severe and life-threatening condition and should not be left in the home, which often causes more harm by delaying the proper treatment. However, the use of home remedies alongside prescription drugs is beneficial. Some home remedies helpful for oesophageal thrush are probiotics (e.g., cottage cheese and yoghurt), prebiotics (poorly digestible foods) to restore the balance of microflora and gentian violet, a dye produced from coal tar that could be swabbed (should never be engulfed).
Antifungal drugs are available as oral tablets or intravenous infections to treat thrush. Mild cases respond to oral drugs, and severe cases need intravenous therapy. The drug of choice is fluconazole, which is the doctor's first choice. If this not works, other drugs like nystatin, itraconazole, voriconazole and amphotericin B are used. Posaconazole (Noxafil) is effective in severe and refractory cases. The treatment usually is last for 2-3 weeks. Some severe cases need hospitalization for proper treatment and monitoring.
With proper treatment and management, it should resolve in 7-14 days or 21 days at the most. The refractory and severe cases need treatment for 2-4 weeks. Any longer duration means some underlying disease and needs hospitalization.
4. Breastfeeding thrush (Candida albicans mastitis in the breastfeeding women)
Breastfeeding thrush, or the yeast infection of nipples, is common in breastfeeding mothers and has repercussions for the health of both mother and baby.
Figure 4: Breastfeeding thrush causes pain in the nipples.
Just like other types of thrush, it is also caused by Candida species. The spores of this yeast and others reside on the skin. During breastfeeding, the warmth and humidity on the nipples create favourable conditions for their growth. The excessive growth of yeast causes infections of deep layers of the skin. Cracked and damaged nipples have perfect conditions for the growth and development of yeasts. Recall that many babies experience several episodes of oral thrush in the first few months. During breastfeeding, there is a chance that the fungus reaches the breast of mothers. Similarly, the infection also passes from mother to baby.
Antifungal drugs are used for treatment. These drugs are available as ointments, gels and creams and are applied directly on the nipples. The commonly available antifungal drugs are nystatin, clotrimazole and miconazole; some preparations are available over the counter. In severe cases, doctors often recommend using oral antifungal drugs like fluconazole. To relieve pain, anti-inflammatory drugs are recommended, e.g., steroid creams. If the baby develops oral thrush or already has, the mother and baby's treatment is needed. If the baby has developed thrush, breastfeeding should be continued as usual.
Breastfeeding can also be continued if the baby has not developed thrush yet. However, some precautions must be followed, like good hygiene, disposable nursing pads, regularly sterilizing the breastfeeding equipment and following the treatment guidelines. The infection goes away in 1-2 weeks with proper antifungal treatment. However, if it takes longer, be patient and wait for more days. The fungal infections are often very refractory to treatment and reoccur within a few days of recovery. However, if the symptoms persist for long, consult the doctor for treatment.
5. Invasive Thrush
It is a severe and potentially fatal fungal infection that occurs when the yeast crosses the physical barriers of the body to reach blood circulation. From the blood circulation, it reaches and establishes in various organs like kidneys, heart, brain, bone, spleen and eyes. Without proper diagnosis and treatment, it is life-threatening. The establishment of yeast infection in the kidney, heart valves, liver and brain is sometimes fatal. The death rate due to invasive candidemia is estimated to be 19-24%.
Figure 5: Invasive candidiasis cause the generalized symptoms of diseases.
The most critical fungal species causing the invasive thrush are Candida albicans, Candida glabrata, Candida parapsilosis, Candida Krisei and Candida tropicalis. Some other species, like Candida dubliniensis, Candida lusitaniae and Candida guilliermondii, have a minor role. The identification of species is essential for targeted therapy.
For treatment, hospitalization is required and involves the injection of antifungal drugs into the bloodstream. Various antifungal drugs are available, like micafungin, fluconazole, caspofungin, amphotericin B and anidulafungin, and the choice depends upon the factors like age, severity and location of infection and status of the immune system. Continuous treatment for 1-2 weeks is typically enough to get negative blood cultures. Sometimes, a prolonged treatment is required in severe cases.
6. Cutaneous Thrush
Also known as cutaneous candidiasis, it is a fungal skin infection. It occurs whenever the warmth and wet skin create favourable conditions for yeast growth, which is among the normal microflora of the skin.
Figure 6: Cutaneous thrush causes irritation and itching.
It develops on any area of the skin. However, the most common sites are the skin folds where the humidity is trapped, and these areas are also warm. So, the most susceptible areas are the groin, armpits, under and between the breasts and the fingers of hands and feet. Some other rare sites are corners of the mouth, nail edges and inside of the nails. Many yeast species are involved, but the most common is Candida albicans, responsible for 80-90% of the cases. Other species like Candida glabrata, Candida parapsilosis, Candida tropicalis and Candida krusei also cause infections in immunocompromised people.
Along with the causative yeast, various other risk factors increase the risk of developing cutaneous thrush-like tight-fitting clothes, warm weather, poor hygiene, prolonged use of undergarments, obesity, excessive and unnecessary use of antibiotics, prolonged use of corticosteroids and other immunosuppressant drugs, pregnancy, diabetes and continuously damp skin. Babies develop it on the buttocks as the diaper, particularly the wet one, provides an ideal environment for yeast growth.
It is prevented and treated by home remedies, lifestyle changes and OTC and prescription drugs. Home remedies like proper hygiene, regular washing and drying, lifestyle changes to control blood glucose levels, and engaging in regular physical exercises are helpful. The persistent and severe cases need antifungal drugs applied as cream or gel. The OTC creams containing drugs like miconazole, clotrimazole and tioconazole are helpful to kill the fungus on the skin and curb its spread. If the OTC treatments don't work, patients should consult the doctor for prescription drugs like ketoconazole and Nystatin.
Oral antifungal drugs are used if the infection has spread from the skin to the other areas of the body, and injectables are used if the yeast has entered the blood. Cutaneous candidiasis is responsive to treatments and recovers quickly without complications in 1-2 weeks. However, depending on the severity of the infection and immune status, it takes from a few days to a few weeks. The infection often reoccurs in people with weak immune systems and need a complete treatment plan.
What are the common Causes of Thrush?
Thrush, whether oral, genital, cutaneous or any other form, is caused by various fungus species. The fungus (yeast) is not harmful, and various internal and external risk factors create favourable conditions for fungal growth. These causative risk factors are;
- Pregnancy: Pregnancy is a period of significant physiological changes and stress, and pregnant women are more likely to develop vaginal or oral thrush. It is due to the changes in the levels of hormones, particularly oestrogen. The studies have found that prevalence
- Corticosteroids: These medications, e.g., prednisolone, betamethasone and dexamethasone, are used to treat pain and inflammation and are also used during autoimmune conditions and allergic reactions. These drugs weaken the immune system and allow the fungus to proliferate.
- Smoking: Smokers have a higher risk of oral thrush than non-smokers because cigarette smoke disrupts the integrity of epithelial cells and the normal microflora of the mouth.
- Medical conditions: There are several metabolic and infectious diseases like diabetes, cancer, HIV/ AIDS, organ transplants, autoimmune diseases like lupus and rheumatoid arthritis etc., which disrupt normal physiology and depress the immune system.
- Weakened immune system: Immune system controls infections, and having a weakened immune system lowers the ability of the body to ward off natural biological challenges, causing an increased risk of many diseases, including thrush.
- Poor oral hygiene: Poor oral hygiene disturbs the oral microflora, causing an increase in the number of harmful bacteria and yeasts. Similarly, using contaminated dentures introduces dangerous bacteria into the mouth, leading to infections like thrush.
- Use of antibiotics: The excessive and long-term use of antibiotics disrupts the normal microflora of the oral cavity and vagina, causing an increased risk of oral and vaginal thrush. Besides killing harmful bacteria, antibiotics also kill helpful bacteria that limit the growth of opportunistic pathogens like Candida.
1. Pregnancy
Pregnancy is a physiological process stretching from conception (fertilization and attachment of zygote in the womb) till the delivery of the baby. The zygote develops inside the uterus during this period. It is characterized by enormous hormonal, physical and emotional changes in the body. These physiological and hormonal changes disturb the immune system and upset the vaginal pH causing it to become more alkaline. The change in vaginal pH alters the balance of oral and vaginal microflora and create a favourable environment for fungal growth.
The higher levels of oestrogen increase the risk of thrush. The risk of thrush in pregnant women is highest during the last trimester (3rd) of the pregnancy when these changes reach a leak. If the symptoms of thrush are noted during pregnancy, the women should consult the gynaecologist and avoid potentially dangerous self-medication and OTC drugs.
2. Corticosteroids
Corticosteroids like prednisolone, betamethasone, dexamethasone etc., are used to relieve pain and inflammation and are frequently used during conditions like bone pain, arthritis, chronic obstructive pulmonary disease (COPD) and asthma. The steroids are included in the inhalers used for respiratory illnesses. These steroids suppress the functions of the immune system, and thus, a small amount of inhaler left in the mouth increases the risk of oral thrush.
Likewise, corticosteroid creams, ointments, gels and suppositories are used in vaginal infections (?) to relieve pain, itching and redness in the reproductive organs. The oral and vaginal use of corticosteroids disrupts the natural microbiological balance of the oral cavity and vagina, increasing the risk of oral and vaginal thrush. The prevalence of oral thrush in people using systemic glucocorticoids was 43.3% compared to 11.67% in non-users, according to a study conducted by Jia-ling Xiao and his colleagues in 2020.
3. Smoking
Cigarette smoke has many dangerous chemicals like lead, arsenic and carbon monoxide that negatively influence the cells inside the mouth and the beneficial bacteria that maintain the microbial balance inside the oral cavity. Therefore, the risk of bacterial, fungal and viral infections is higher in smokers than non-smokers. During the development of oral thrush, the causative yeast (Candida albicans, in most cases) invades and adheres to the host tissues. The chemicals in cigarette smoke interfere with the attachment and adhesion of Candida albicans resulting in biofilms inside the mouth and the proliferation of fungal growth.
Smokers often experience dry mouth due to decreased saliva production, which causes damage to the oral tissues. This damage allows the fungus to adhere to the tissues and cause thrush. Smoking also weakens the immune system, reducing the ability of the body to fight infections. It also disturbs the levels of hormones, resulting in a higher risk of vaginal thrush. So, smokers are at risk of higher levels of other types of thrush, not only oral thrush.
4. Medical Conditions
Several medical conditions also increase the risk of developing thrush. These include metabolic diseases like diabetes and infectious diseases like cancer and HIV. Yeasts need sugar to grow, and poorly controlled and higher levels of glucose in the blood create a favourable environment for yeast growth. Hypoglycemia also influences the immune system by suppressing the functions of the immune system. Consequently, the risk of thrush in people with diabetes was 22.1% compared to 9.7%, according to a study published in the Indian Journal of Dental Research in 2021.
Likewise, various conditions affect the immune system and disrupt the natural homeostasis of the body like autoimmune diseases (inflammatory bowel disease, lupus, rheumatoid arthritis etc.), having an organ transplant in the recent past, chronic kidney or liver diseases, cancers and immunosuppressive diseases like HIV/AIDS.
5. Weakened immune system
Yeast infections in the mouth, vagina or anywhere in the body indicate that the immune system has failed to eliminate disease, and medical intervention is required. The weakening of the immune system allows the fungus to adhere to the tissues and cause thrush. The immune system protects the body from infections. Whenever the fungus attaches to the body, the immune system recognizes it. It mounts an immune response by activating immune cells, which either kill the fungus directly or produce antibodies that neutralize the fungus and fungal spores.
In case of milder immune system weakness, the body takes longer to recover from the fungal infections. In severe immune deficiency, persistent and more serious fungal infections (invasive thrush occurs) occur that are often fatal. So, any factor causing a weakened immune system, like poor nutrition, immunosuppressant drugs, immunosuppressive diseases (like HIV), smoking and chronic illnesses, causes an increased risk of developing thrush. Consequently, the risk of thrush is much higher (more than 90%) in HIV patients.
6. Poor Oral Hygiene
Poor oral hygiene, like using contaminated dentures, irregular brushing routine, and oral diseases like stomatitis (the inflammation of the mouth), results in the breakage of the integrity of oral mucosa and allow the fungus to adhere and develop thrush. The use of oral dentures introduces many germs inside the mouth.
Candida is a typical inhabitant of 45-65% of normal and healthy people, and this percentage rises to 60-100% in the people who use dentures. In addition to a higher prevalence of yeast in people with poor oral hygiene, it also increases the risk of more dangerous and often fatal invasive candidiasis. Poor oral hygiene also causes the buildup of bacteria and plagues in the mouth, which form a favourable environment for fungal growth.
7. Use of Antibiotic
Antibiotics treat bacterial infections and prevent secondary bacterial infections in case of viral and fungal infections. Antibiotics are used to kill harmful bacteria, but they have no way of knowing whether the bacteria are harmful or valuable and kill indiscriminately. This killing depletes the bacteria population, which keeps the fungal growth in check. Although they don't interfere with the immune system, excessive use causes under activation of the immune system.
What other lifestyle factors increase the risk of Thrush?
Thrush is ubiquitous; one-fifth of men and women and more than one-third of under aged children experience some form of thrush at some point in their life. Although some risk factors determine the risk, it needs to be clarified why some people have more chance than others. Alongside medical and biological reasons, some lifestyle risk factors influence the development of thrush. These are;
Clothing: The breathable and light dresses and undergarments allow the moisture to evaporate and prevent water accumulation, which is required for fungal growth. Synthetic materials like polyester and nylon are not breathable and trap moisture, creating a favourable environment for fungal growth. The risk of cutaneous thrush is higher in winter months because heavy garments don't allow enough ventilation. However, the risk of vaginal thrush is higher in hot and humid weather.
Cleaning and washing routine: The washing routine is essential as it is noted that regularly washing the mouth or vagina with simple water lowers the risk of thrush. In contrast, using scented body washes and gels disturbs the vaginal pH, often altering it to benefit the Candida. Proper oral and skin care reduces the risk of oral and cutaneous thrush.
Use of contraceptives and lubricants: Some studies have noted that combined hormonal contraceptive pills increase the risk of thrush. Because these pills have estrogen, it increases the survival rate and growth of yeast. Likewise, using intrauterine devices (IUDs) introduces infections into the vagina. So, in case of repeated incidences of thrush, carefully considering the choice of contraceptive methods is very important.
Likewise, using spermicidal lubricants also increases the risk of developing thrush as these products have ingredients (like nonoxynol-9) that not only kill the sperm but also disturb the vaginal microbiological balance by killing the beneficial bacteria.
Stress: Chronic stress reduces the ability of the body to fight infections. Stress increases cortisol levels. This hormone negatively influences the immune system by blocking the T cells. These factors allow infections, including the thrush, to take hold. Chronic stress creates conditions that allow the Candida to multiply and excel in the competition against other germs. So, in case of repeated incidences of thrush, it is essential to look at the lifestyle to see if there is some chronic stress.
Diet: Candida and other opportunistic pathogens need sugars for proliferation and so diets rich in sugars like refined grains, pasta, cookies, candies, cakes, and white bread increase the risk of infections. The studies have noted that switching to low-sugar diets keeps the yeast population in check by starving them of sugars. But, any dietary modifications should be consulted with the doctor and nutritionist to avoid the risk of unnecessary nutritional deficiencies.
Poor sleep: Proper and healthy sleep is required for the proper functioning of the immune system, and healthy sleep allows the body to maintain optimal health balance by repairing itself. Poor sleep results in poor immunity and the proliferation of harmful bacteria, which causes the vaginal and oral pH to change, making it more favourable for fungal growth.
Careless use of drugs and medications: As the excess use of steroids, antibiotics, and oral contraceptives increase the risk of developing thrush, it is essential to be careful with the choice of medications. Birth control pills with estrogen increase the risk of thrush and must be replaced with oestrogen-free tablets. Similarly, the indiscriminate killing of bacteria by antibiotics also allows fungal infections to take hold by killing the competitors. The steroids suppress the body's ability to fight the infections. So, if the symptoms of thrush are noted while taking certain medications, it is essential to consult the doctor and add some probiotic foods to support the normal microflora.
All of the people exposed to these issues do not develop fungal infections, but these factors nevertheless increase the risk.
What are the hormonal factors that contribute to thrush?
Hormones control all body functions, hormonal changes cause changes in the physiology and chemistry of the body, and some of these changes contribute to the development of thrush. Almost 50% of cases of mucocutaneous thrush have some endocrine cause. The following hormones have a role in the development of thrush;
Oestrogen: Oestrogen is responsible for developing female reproductive organs. Higher levels of this hormone influence the vaginal pH. High oestrogen levels increase the glycogen in the vaginal cells, thus allowing the fungus to proliferate. The risk of thrush is higher in women taking combined pills containing oestrogen.
Cortisol: Cortisol is produced by adrenal glands as the body faces stress. Higher cortisol levels suppress immune functions, allowing the Candida species to take hold. So, chronic stress is a severe predisposing factor to thrush.
Progesterone: This hormone has a role in pregnancy and regulating the menstrual cycle. Its elevated levels create a favourable environment for fungal growth. It is one of the reasons why pregnant females and females using progesterone pills have a higher risk of developing thrush.
Thyroid hormones: The thyroid hormones like T3 and T4 regulate energy production and metabolism. The lower thyroid hormone levels suppress the metabolism and the immune system's functions. That's why people with hypothyroidism are more susceptible to thrush.
Insulin: Insulin regulates blood sugar levels, and its lower levels, as seen in people with diabetes, result in higher blood glucose levels. Very high levels of insulin, as seen in people with uncontrolled diabetes, create conditions that are favourable for fungal growth.
Androgens: Androgens are the male hormones that are also produced in small amounts in females. Higher androgen levels, as seen in some diseases like PCOS, influence the vaginal environment and make it more susceptible to yeast growth.
Growth hormone (GH): This hormone controls growth and development. Studies have found that its lower levels influence growth and development and suppress the immune system, making a person more prone to infections, including thrush. Children deficient in growth hormones experience more episodes of thrush.
Using some drugs like corticosteroids and hormones like birth control pills also alters the balance of hormones in the body and influences the immune system to increase the risk. Certain medical conditions that affect the hormones, like Cushing's syndrome (high cortisol levels) also disturb the levels of hormones. However, it should be noted that hormones do not cause thrush directly; they increase the risk in combination with other factors.
Does stress cause thrush?
Yes, stress is one of the risk factors of thrush. Stress negatively influences the immune system by increasing the production of cortisol, thus reducing the ability of the body to control infections. Stress negatively impacts eating patterns, habits and hygiene protocols, and a stressed person is likely to have poor eating habits and poor hygiene. Some people use comfort food which is often sugary snacks and also neglects oral hygiene, which creates a favourable environment for fungal growth in the mouth. Likewise, stress increases the risk of vaginal and cutaneous thrush by influencing reproductive hormones and causing ignorance of reproductive hygiene. A weakened immune system due to stress increases the risk of invasive candidiasis.
Can a poor diet cause thrush?
Yes, poor diet is a significant risk factor for thrush. A poor diet rich in sugars, processed foods, refined grains and unhealthy snacks allows fungal growth by providing them with food. Likewise, a poor diet is likely to be deficient in essential nutrients like essential amino acids, proteins, minerals and vitamins, which are necessary for immune functions and lower the ability of the body to ward off infections. A poor diet and poor dietary habits negatively influence oral hygiene allowing the trapped food particles to stay in the mouth and serve as a food source for the fungus. So, like stress, a poor diet is not a direct cause of thrush; it just adds to the risk.
Can sexual activity cause thrush?
Yes, sexual activities are a considerable risk factor for genital candidiasis, particularly in women. Sexual activities, particularly with infected partners, introduce new germs into the vagina, disturbing the microbiological balance. If the male partner has thrush on the external genitals, it can enter the vagina and cause vaginal thrush if other risk factors are present. Similarly, an infected female also transfers the infection to her male partner. Additionally, sexual practices like using poor-quality condoms, spermicidal lubricants and engaging in oral sex increased the risk of thrush. The spermicidal contraceptives disturb the vaginal microbiological balance by killing the beneficial bacteria that keep the population of harmful bacteria and fungi in check. So, sex is not a direct cause, but it adds to the risk in the presence of other risk factors.
What are the Signs and Symptoms of Thrush in Men?
The signs and symptoms depend upon the type of thrush and the nature of the locations.
In the case of oral thrush, the following signs are noted;
- Raised white lesions develop on the cheeks, back of throat, gums, tonsils, and tongue. These lesions cause pain, redness and irritation.
- The angular cheilitis (the redness and cracking on the corners of the mouth) appear with a cotton-like feeling and occasional loss of taste.
- Creamy white pseudomembranes develop that cover the surface of the tongue, throat, roof of the mouth and inner cheeks. These membranes are a mixture of fungal elements, debris and dead cells, appearing as yellowish and whitish plaques.
- The scrapping of these pseudomembranes reveals inflamed and reddened mucosa underneath.
- Burning sensation in the oral cavity.
- Difficulty in swallowing.
- The denture stomatitis develops, causing pain, redness and irritation under the dentures.
- In severe cases, the infection speeds to the oesophagus causing painful swallowing and fever.
Invasive thrush: Sometimes, the infection spreads through the blood into other body organs (invasive candidiasis). In that case, generalized signs like fever, chills, hypotension, abdominal discomfort and pain, vomiting and nausea, stiffness and pain in the joints, rapid heartbeat, weakness, loss of appetite and nervous symptoms like poor concentration and confusion also appear.
Cutaneous thrush: The signs of cutaneous candidiasis are more localized on the skin due to deep and penetrating lesions. These include cracking, flaking and scaling of the skin, soreness, burning and itching in the affected area, pinkish to reddish rashes, blisters or raised bumps and foul odour in severe cases.
Genital thrush: The most common Candida infection in males is the genital thrush. It results in the inflammation of the glans penis (tip of the penis), known as balanitis. It causes painful symptoms like burning, redness and itching on the head of the penis and also under the foreskin, cottage cheese-like discharge from the infection site, unpleasant odours, hardening of the foreskin, difficulty in pulling the skin, irritation and pain during sex and urination and the appearance of blotchy rashes causing white patches and small bumps.
What are the Signs and Symptoms of Thrush in Women?
The signs and symptoms of cutaneous, oral, and invasive thrush are common in men, women, and children. The females experience vulvovaginal candidiasis, characterized by the following signs;
- The vaginal thrush is asymptomatic in 20% of patients.
- Redness, swelling, itching and irritation around and inside the vagina.
- Stinging and burning sensation during and after urination
- Discomfort and pain during sex
- Thick whitish or creamy discharge resembling cottage cheese
- Sometimes, the vaginal discharge is watery, with soreness and pain in the vagina
- Some additional signs are reported in the complicated cases, like, extensive itching, redness and swelling leading to sores, cracks and tears, repeated fungal infections throughout the year, infections by novel species of fungus and little or no relief from the antifungal drugs.
What are the Signs and Symptoms of Thrush in Children?
Signs and symptoms of thrush in children depend upon the organ where the thrush develops and are experienced differently for each child. The most common symptoms in children are;
- In the case of cutaneous thrush, the lesions develop in the navel and the skin folds. These lesions cause burning, itching, pimples, rashes and the formation of white patches that ooze out clear fluids.
- If the thrush develops in the vagina of young girls, the signs are burning and redness in the external genitals, itching and yellow or white vagina discharge. In young male children, the thrush developing on the penis causes signs like redness, painful rashes and scaling.
- The oral thrush (the most common one in children) causes pain and white patches on the inside areas of the cheeks, the top of the mouth, and the tongue. Tiny cuts and cracks appear on the corners of the mouth.
- The children also experience the fungal infection of the nail buds (paronychia), causing yellow or white nails, pain, swelling, pus and ultimately, the separation of nails from nail buds.
How long do the symptoms of thrush last?
The duration of thrush depends upon factors like the nature and severity of the infection, whether it was treated or not, and if treated, what treatment was used. Milder cases resolve spontaneously within a week, while more complicated issues take longer. The symptomatic treatment provides quick relief from the symptoms like foul discharges, burning, itching and redness and causes some people to leave treatment.
However, it is essential to complete the treatment until the infection has cleared completely. The untreated cases of thrush persist for several weeks and even months and often spread to other body parts, mainly in patients with a weak immune system. This invasive candidiasis causes severe complications and even death. Generally, if the symptoms do not improve after 2-3 weeks of regular treatment, it is better to consult the doctor.
How can you tell if a skin rash is caused by thrush?
The thrush causes body rashes. These rashes develop as moderate temperature and high humidity create suitable conditions for fungal growth, allowing the fungus to penetrate deep into the skin. The fungal penetration and the resulting immune reaction cause severe rashes. Two common types of rashes reported due to candidiasis are candidal diaper rashes, which develop on the baby's diaper area, and body rashes, which develop anywhere on the body where fungus grows.
These rashes occur in people who have poor immune systems, use antibiotics or have diabetes. These rashes are similar to those caused by autoimmune conditions and allergic reactions. The following signs show that the skin rash is due to thrush;
- The area is red, scaly, itchy and raised and has small pimples and bumps.
- The rashes are developing in moist and warm areas like armpits, groin etc., and are not developing in dry and ventilated areas
- The rashes are causing discomfort, burning and itching.
- A noticeable odour is produced from rashes.
Can thrush cause fever or chills?
Yes, fever and chills are observed in invasive thrush. In most cases, thrush is a localized infection limited to the mouth, vagina, skin and nails. Still, in rare cases, particularly in people with Immune deficiency, the fungus reaches the blood to cause a systemic infection (candidemia). Sometimes, it also happens that the thrush is accompanied by other systemic bacterial or viral infections which cause fever and are often overlooked as candidemia. So, the patients need to consult the doctor for differential diagnosis.
Can thrush cause pain during urination?
Yes, thrush causes pain during urination if the infection has spread to the urinary tract. The common symptoms in these situations are burning and pain during urination. Pain during urination could be due to urinary tract infections (UTIs) or yeast infections. Although both conditions are different, there are some common symptoms. If a male experience pain during urination, it is a definite sign of UTIs, but in females, there are two possibilities, UTIs or vaginal thrush.
The other urinary system symptoms in yeast infections are pain during and after sex, itchiness, pain and swelling in the vulva and vagina and oozing out milky, thick cottage cheese or odourless discharge from the reproductive organs. It is important to note that ascending fungal infections from the lower reproductive tract also cause UTIs. So, having pain during urination should arouse the possibility of both thrush and UTIs.
How is thrush diagnosed?
Like other infections, the fungal infection is diagnosed through a combination of approaches like medical history, physical examination and laboratory testing.
Physical examination
The physical examination is beneficial for diagnosing cutaneous candidiasis and other types. During a physical exam, the doctor inspects the affected area like skin, mouth and vagina using eyes or visual aids like a magnifying glass. The signs of thrush, like white patches, swelling, redness and pain, are detectable visually. These signs also provide indications to the healthcare providers to differentiate it from other similar conditions like allergic reactions, stomatitis, vaginitis etc.
Medical history
Healthcare professionals often ask patients to self-describe the signs and symptoms. The information about other current or past diseases and the medications used to treat them is beneficial. Questions about sexual life, nutrition, lifestyle and past fungal infections are also asked.
Endoscopy
During endoscopy, a tube is inserted into hollow organs like the oesophagus and vagina to look for thrush lesions. However, this method is not favoured as it causes the spread of infection.
Microscopy
During microscopy, the pathologists take swab samples from the mouth or other affected organs, prepare slides and examine it under the microscope to identify the fungus or fungal spores.
Culture
During culture, a sample is taken from the affected area, and the fungus is grown on artificial media and identified. The swab samples are collected from the skin, mouth, vagina or blood sample and are used to detect invasive candidiasis. The sample is transferred to the artificial media that supports the fungal growth. Following the injection, the samples are incubated in an incubator where optimum conditions for fungal growth are provided. After incubation, the samples are examined for fungal growth. Cultures are highly accurate but are very time-consuming and need technical expertise.
Blood tests
Blood tests like CBC are used to diagnose any infection. Blood tests are helpful for the diagnosis of invasive thrush. The blood tests detect the segments of fungal hyphae or the antibodies produced by the body in response to these segments.
Does thrush need a Blood Test to diagnose?
Yes, blood tests help diagnose invasive candidiasis, which is a severe type of thrush and has systemic implications. For most types of thrush, blood tests are not required. But, the fungus reaches the blood in the invasive type, and blood testing is helpful. In such cases, mostly the blood cultures are done to see the presence of fungus, and negative blood culture indicates that the infection has been eliminated from the body. The other blood tests used for thrush are;
Candida albicans germ tube antibody test (CAGTA-test): This test detects the thrush caused by C. albicans but is less sensitive to detecting other fungal infections.
Mannan and anti-mannan antibody test: Mannan is a carbohydrate in the fungal cell wall. This carbohydrate or antibodies produced in response to it are used to diagnose the invasive thrush.
Polymerase chain reaction (PCR): This test detects the segments of the fungal genome in the blood by amplification. Various commercial PCR-based tests are available to detect all five causative species, i.e., C. krusei, C. tropicalis, C. parapsilosis, C. glabrata and C. albicans. These tests are particular but need technical expertise and apparatus and are expensive.
(1,3)-β-D-glucan test (BDG-test): The BDG is a carbohydrate in the fungal cell wall. Like mannan testing, it is also helpful to diagnose the invasive thrush. However, as many fungal species have BDG, this test doesn’t help identify species.
T2Candida panel: This test diagnoses the invasive thrush by identifying all five common Candida species in the blood.
Since none of the blood tests are 100% accurate, the doctors use a combination of tests and physical examination to establish the final diagnosis.
Is thrush contagious?
No, it is not considered to be contagious in the traditional sense. The contagious infectious diseases are transferred from one person to another under ordinary conditions through respiratory droplets, touch, sexual contact or use of clothing and utensils. The Candida species are not easily transferred from one person to the others and need exceptional circumstances for transmission. For example, it is transferred from the infected sexual partner to the other partner or from the mother to the baby and vice versa only if the other person has the required conditions for fungal growth like moderate temperature, high humidity and poor immunity. The rate of transmission is minimal as compared to the traditional contagious disease.
What are Treatments of Thrush?
The treatment of thrush depends upon the causative agents, the presence of risk factors, the location of lesions, the severity of the disease, the immune system of the patients and the presence or absence of other secondary infections. The standard treatment options are antifungal creams, ointments and lotions, over-the-counter drugs, oral prescription antifungal drugs, systemic antifungals in case of invasive thrush, intravaginal suppositories and antibiotics to treat secondary bacterial infections.
Antifungal drugs are used to treat thrush. These drugs are available as topical preparations applied directly on the affected area or as oral pills that are engulfed and work systemically. Some lozenges containing antifungal drugs are available that curb the growth of fungus. The first treatment is topical preparations; if they don't work, the doctor’s shift to oral drugs, and in severe cases, the IV drugs are injected, particularly for invasive thrush. The healthcare providers also identify the predisposing factors for a more efficient cure.
The typical duration of treatment is 10-14 days, and the patients should consult the doctor if it doesn't work. The treatment must be continued for refractory cases for 28 days, depending upon need. The standard line of action for different types of thrush is;
Oral Thrush: For oral thrush, a suspension of different antifungal drugs (e.g., nystatin oral suspension and clotrimazole troches) is applied on the mucus membranes, swallowed or swished in the mouth. The nystatin oral suspension has 100,000 units/ mL, and 5 ml of rest is used four times daily. It is swallowed after several minutes of swishing. Sometimes, the doctors also recommend miconazole gel. This protocol is enough for ordinary and uncomplicated cases. However, oral antifungal drugs are prescribed for complicated and severe infections.
Vaginal thrush: For vaginal thrush, different antifungal treatments are applied on or into the vagina as ointments, creams or suppositories. These local medications are coupled with oral drugs for fast recovery. A typical therapy is to use intravaginal azoles for one week or three doses of 150 mg fluconazole every third day. Patients with severe and recurrent infections also benefit from weekly fluconazole for six months.
Cutaneous thrush: The topical preparations are enough for cutaneous thrush, and the oral and systemic antifungals are rarely needed. The topical drugs are sometimes coupled with anti-inflammatory and antibacterial drugs to reduce the risk of secondary infections and relieve pain and inflammation. The most common topical preparations contain miconazole, nystatin and clotrimazole, and regular use ensures complete recovery. A review by Taudorf and his colleagues in 2019 found that these drugs provide cure rates of 73-100%.
Invasive candidiasis: For invasive candidiasis, systemic therapy is required. The choice of treatment depends upon the severity of the condition, the patient's age, immune status and other concurrent infections. The first treatment of choice for adults is the echinocandin drugs (like anidulafungin, micafungin or caspofungin) given through the intravenous route. For youngsters, doctors use amphotericin B, fluconazole or other antifungal drugs that are also useful for all patients.
The treatment should continue for two weeks after the resolution of clinical signs and until the yeast has been eliminated from the body (negative blood culture test). More prolonged treatment is required if the infection has spread to other areas like the central nervous system, heart, heart valves, joints or bones.
Thrush treatment during pregnancy: The treatment of yeast infection follows the same protocol. However, some antifungal drugs like ketoconazole, griseofulvin and flucytosine are embryotoxic and teratogenic (cause abnormal development of baby). Likewise, iodides are associated with congenital goitre and should be avoided in pregnancy. As a general rule, any treatment during pregnancy should be discussed with the doctor.
For all other types of thrush, the symptoms begin to improve after 3-5 days of regular treatment. However, treatment should not be discontinued as the fungus is tough to kill, and incomplete treatment is likely to result in treatment failures and the reoccurrence of infection.
How long does it take for thrush to clear up with treatment?
The duration of treatment depends upon factors like the nature and type of treatment given, the disease's type and severity and the immune system's status. Proper treatment usually ensures complete recovery in 1-2 weeks. However, it is essential to note that the fungus is very resilient, and its spores are tough to kill. So, it is recommended to continue to use antifungal drugs for 1-2 weeks more after the resolution of the symptoms to ensure full recovery and avoid relapses.
The type of disease and the lesions' location also influence the disease's duration. For example, typical treatment plans like topical antifungal preparations (containing Nystatin, clotrimazole etc.) and systemic antifungals in case of more severe infections and poor immunity ensure recovery in 1-2 weeks. The treatment should continue for many weeks for complicated cases for a full recovery. Symptoms improve after 3-4 days of use. However, it is strongly advised not to leave treatment at this stage.
In the case of vaginal thrush, the typical treatment protocols provide results in 2-3 days, and treatment should continue for more days for an effective cure. The invasive thrush treatment must be carried out for several weeks until a negative blood culture test is obtained. The uncomplicated cutaneous thrush responds swiftly to the local drugs and resolves within days to weeks. However, it should be kept in mind that there are person-to-person variations and many times, there are unexpected factors, so the patient should consult the doctor regularly and follow his directions.
What are the possible side effects of antifungal medications used to treat thrush?
The side effects of antifungal drugs depend upon the type and dosage of the drug being used. The common side effects are stomach upsets, abdominal pain, diarrhoea, skin rashes, and burning and itching at the application site. The rare side effects are jaundice (liver damage) and severe allergic reactions causing symptoms like rashes, anaphylaxis, peeling of skin and blisters.
The patients need to be aware of the side effects of individual thrush medications and report them to the doctor. These include;
- Amphotericin B: The common side effects are nephrotoxicity (deterioration of kidney functions due to the toxic impacts of drugs, medications and chemicals), hypomagnesemia (lower serum magnesium levels), hypokalemia (lower serum potassium levels) and suppression of bone marrow. Nephrotoxicity is the most common side effect, while occasionally, bone marrow suppression occurs due to long-term use leading to symptoms like anaemia. The kidney and liver parameters of the patients receiving long-term therapy should be monitored for early response.
- Azole antifungal drugs: The azole antifungals like voriconazole, posaconazole, itraconazole, fluconazole and isavuconazole etc, are emerging in the market. These are associated with side effects like;
- Fluconazole: Rashes, gastrointestinal discomfort, occasional toxicity (mainly when heavy doses are used) leading to symptoms like alopecia, anaphylaxis, Stevens-Johnson syndrome and hepatic toxicity and congenital fetal anomalies.
- Isavuconazole: Hepatitis, gastrointestinal disturbances and lowered QT interval (poor cardiac health).
- Itraconazole: GI upsets, oedema, hypertension, hypokalemia, hallucinations, hepatitis, allergic reactions and occasional heart failure.
- Posaconazole: Hepatitis and increased QT interval.
- Voriconazole: Dermatological reactions, hallucinations, visual disturbances, increased QT interval and hepatotoxicity.
- Echinocandins: These drugs include micafungin, caspofungin and anidulafungin. They are associated with side effects like rashes and hepatitis.
- Flucytosine: The common side effects are enterocolitis, hepatotoxicity, and bone marrow suppression, causing leukopenia and thrombocytopenia.
These effects could be temporary or permanent, and the patients need to cooperate with the doctor for early detection and treatment. The prolonged self-medication or the prolonged use of OTC drugs is strongly guarded.
Can you purchase antifungal medications for thrush at an Online Pharmacy?
Yes, the pharmacies registered with the General Pharmaceutical Council (GphC) are authorized to sell antifungal drugs online to the patient. To purchase the medications, the patients must consult the pharmacist or doctor online or complete an online questionnaire. Based on this data, the doctor/ pharmacist make a judgment and generates the prescription, which is forwarded to the online pharmacy that delivers the prescribed medications at the patient's location. However, self-medication of skin diseases is not recommended. The patients must consult the doctor or dermatologist for better assessment as the signs and symptoms of many skin conditions are very similar, and self-medication is often counterproductive.
Can natural remedies be used to Treat thrush?
Sometimes, it is possible to treat fungal infections through OTC drugs or home remedies successfully at home. The benefits of natural remedies are self-reported and anecdotal only, and little scientific backing is available. However, they are associated with rare side effects and are preferred by many. The following natural remedies are available.
Boric acid: The boric acid-containing products are available for topical use, and the boric acid-containing capsules are also available for vaginal use. Some doctors recommended that regularly using a 600mg boric acid capsule in the vagina once a day for two weeks provides good results. The results are even better if it is combined with other antifungal drugs. Some preparations are irritant and should be used cautiously.
Probiotics: Probiotic supplements are available at online stores or health pharmacies. Some products are designed specifically for the female reproductive tract and oral cavity. These supplements (either taken orally or inserted into the vagina) help restore the reproductive tract's natural balance of fungus and bacteria. A review by Tiziana Mundula and collegues in 2019 noted that probiotics are helpful in the oral candidiasis particularly for the denture wearers.
Tea tree oil: Tea tree oil (an essential oil) has anti-inflammatory and antifungal properties and is known to kill many species of yeast and fungus. Research supports that using vaginal suppositories containing tea tree oil benefits vaginal infections. Some women have reported the benefits of applying dilute tea tree oil into the vagina through a tampon. It is a natural oil and irritating the skin, so it should be used after dilution with some carrier oil.
Yoghurt: The unsweetened and natural yoghurt is an excellent probiotic containing many beneficial bacterial species that help restore the microflora balance and improve overall health. Many people have reported benefits by eating it orally, applying it inside the vagina or on the area around the vagina. However, plain yoghurt should be used as the added sugars are dangerous and worsen things.
Garlic: Garlic has antifungal and antibacterial properties. It could be added to the food, and many products for topical and vaginal use are also available. A study by Sobitha and colleagues in 2005 found that the regular daily application of garlic paste for 14 days is as effective as clotrimazole solution to treat the symptoms of oral thrush.
Coconut oil: The antifungal properties of coconut oil combat the growth of yeasts, including the infamous Candida albicans. The organic preparations containing coconut oil are available for internal and external use. It could also be used as a carrier for other essential oils for fungal infections.
Oregano oil: The oregano oil (an essential oil) prepared from wild oregano has antifungal compounds like carvacrol and thymol. Its use, both topically and applied inside the vagina (using capsules or a tampon), helps control fungal growth.
These home remedies work for most people; however, some people, like pregnant women, having ongoing fungal infections, people with sexually transmitted diseases and people whose diagnosis is not established yet, should not use them.
Can thrush be prevented?
Yes, it is possible to prevent fungal infection by following the prevention protocols. It is an infection and develops only when the immune system fails to curb its growth or conditions are favourable for fungal growth. Maintaining a healthy immune system and preventing the development of conditions that favour fungal growth helps prevent thrush and other fungal infections.
How to Prevent Thrush?
These protocols and practices help prevent the thrush.
- Maintaining good oral and vaginal hygiene: Maintain the brushing and flossing routine for a clean mouth. Similarly, maintain vaginal hygiene by using safe sex protocols.
- Eat a healthy balanced diet: A healthy and balanced diet provides all essential nutrients to the body and keeps the immune system strong. A balanced diet also deprive the fungus of the food.
- Avoid using chemical-based and irritant products like vaginal douches, bubble baths, scented soaps, and mouthwashes, as they disrupt the natural microbiological balance in the oral cavity and vagina, paving the way for fungal infections.
- Don't allow the affected areas to be consistently wet. The fungus thrives on the wet skin. Using breathable clothes made from natural fibre allows the moisture to escape and doesn't allow moisture buildup for fungal growth.
- Wear loose-fitting and breathable clothes: The tight-fitting clothes prepared from synthetic materials cause moisture buildup, favouring fungal growth. So, breathable clothes like those prepared from cotton are helpful.
- Treat and manage the disease conditions, if any are present. The conditions like cancer, HIV and diabetes increase the risk of thrush; thus, preventing or managing these diseases is helpful.
These precautions help lower the risk of developing thrush, but once it has been established and signs and symptoms are apparent, these practices are of little use, and treatment is required.















 Rated Excellent by 26,523+ Reviews
Rated Excellent by 26,523+ Reviews