Can you still test positive for COVID after 14 days?
.png?v=1673865009975)

Related products

The coronavirus continues to plague humanity well into 2025. The clinical presentation of the disease is variable across different communities and regions. While the usual course of infection is 1-2 weeks, and a negative test after this period is thought to signal the end of disease and cessation of isolation, however, some people continue to test positive after this period.
You may continue to test positive for COVID-19 for several days even if the clinical signs have subsided.
Why is it so? This phenomenon is due to the problems with the individual immunity and sensitivity and specificity of the tests used. Should these people continue to practice isolation until a negative test? The opinions of the medical community are divided. Let's summarise some important facts about it.
Learn more about COVID-19 on our Health Hub.
Are you still positive after 14 days?
A person can be tested positive even if the clinical signs have disappeared for up to 2 weeks. There are multiple reasons for this, however, the introduction of new variants is the most likely cause. These newer variations of the virus has can linger in the body for longer, which means a positive test result may still occur after 14 days.
How does a COVID test work?
The COVID tests are conducted on the blood or the swab samples from your throat or nose. Currently, two types of COVID tests are being used;
Nucleic acid amplification tests (e.g., PCR)
Nucleic acid amplification tests detect the viral genetic material in your body for as long as 90 days after the infection. These tests are conducted in the laboratory and are the most accurate for asymptomatic people. However, PCR tests take a longer time to give results. These tests are used to confirm the positive test results from the antigen tests.
Our Fit to Fly COVID test is a PCR test and gives results within 8 hours. Click here to get your test kit. The user manual in the kit provides all the technical details about the test.
Antigen/ antibody tests
These are rapid screening tests and give results within 15-30 minutes. These tests detect the viral antigens (proteins) or the antibodies produced in response to these antigens in the blood. These tests are good for initial screening but need to be more accurate. Therefore, a negative test should be viewed with suspicion until a second negative test confirms the findings 48 hours later.
A positive rapid test should be combined with clinical signs and symptoms. Some tests have also been developed to detect and quantify the antibodies produced in response to the viral antigens. The antibody levels also reflect the level of immunity. Order one of these antibody tests by clicking here.
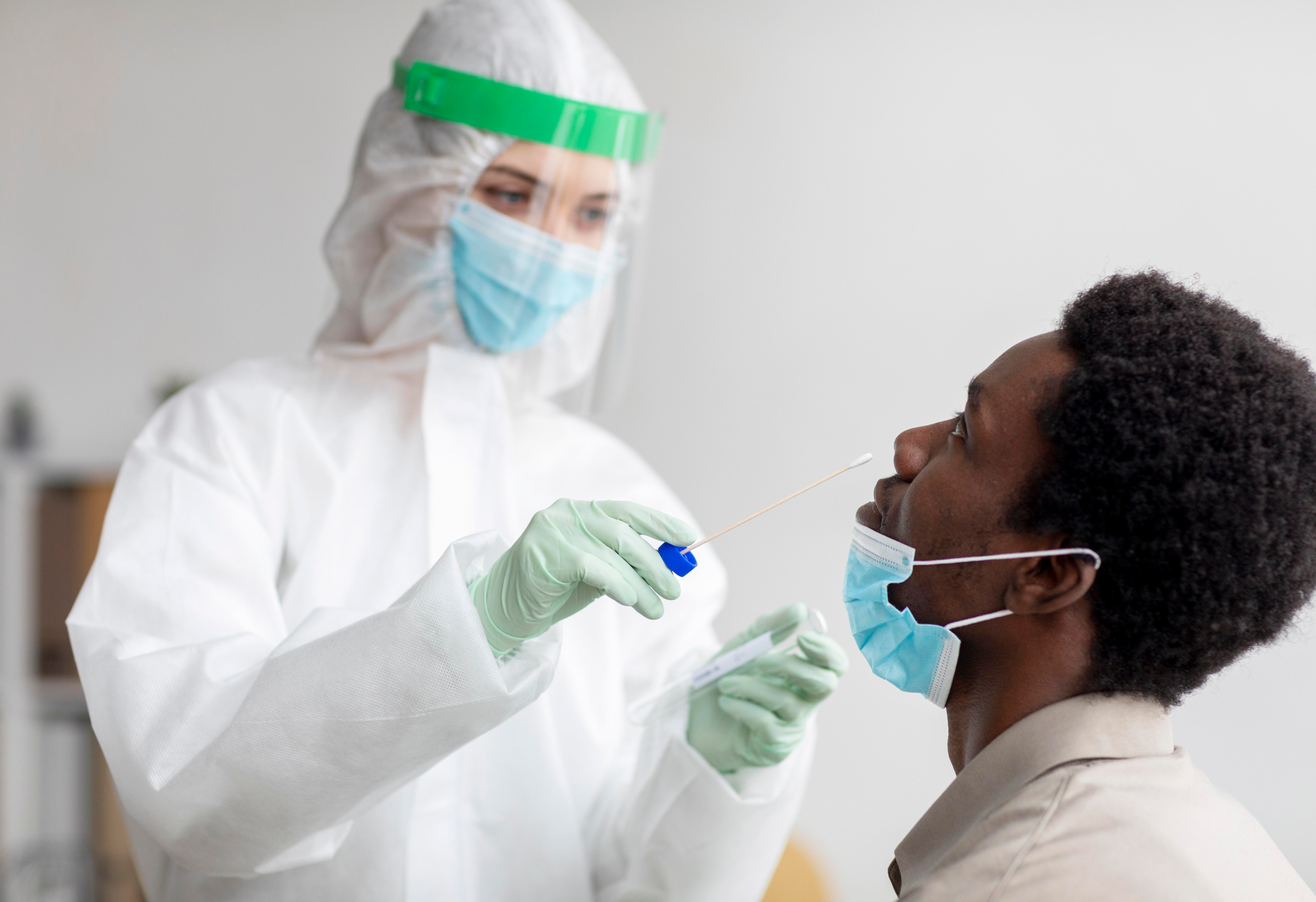
For most patients, the rapid antigen tests are positive for up to 10 days. But, there are still some individual variations. Let's know what are the causes of these variations.
Read more about antigen tests on our Health Hub.
How can a person stay positive for a longer time on rapid tests?
While it is not expected, it is still probable. A lot of factors can cause you to stay positive even after 10 days, e.g.,
Different viral variants
The virus also responds to challenges, giving rise to different variants. The immune system responds differently to different variants. So, these variants also behave differently in rapid tests. Some studies confirm it e.g.,
-
A report published in the New York Times noted that different omicron variants spread quickly within the body and also within the community. The viral levels peak within 5 days of detection (a positive test). However, many people continue to test positive for more than 14 days after the end of the infection.
-
Similarly, another review published in 2022 noted that among the people who tested positive for omicron and developed clinical signs, 20% continued to test positive after 11 days of the appearance of signs and symptoms. It was attributed to the remnants of viral antigens/antibodies in the blood that persisted after the end of the disease.
Similarly, the data is variable for other variants too. According to immunologists and virologists, this variability is related to the variable nature of the human immune system, and it's the variable ability to respond to different these variants and clear them from the body.
The quest for the reason has noted many other factors. Some of these factors are;
A weaker immune system
The immune system is tasked with defending the body from foreign invasions. A strong immune system will fight and eliminate the virus within a few weeks. But, people having weaker immune systems are likely to take much longer to clear the viral load, although some people with apparently good immunity also continue to test positive for a long.
The same is the case for the people who have been vaccinated and have developed good immunity against the virus but are still testing positive for COVID-19.
The degree of viral exposure
The other factor is viral exposure, as it has been noted that a high degree of exposure and a high viral load take much longer to recover. A low viral load doesn't cause symptoms in people with good immunity.
The COVID-19 restrictions were imposed to lower the exposure of the population.
The testing and sampling technique being used
The sensitivity of the test being used and the sampling technique employed also have a role. The use of nasal swabs is more likely to give a positive test than the use of throat swabs. It is due to more viral load in the respiratory airways. Some practitioners used both nasal and throat swabs for better results.
It was noted by a study published in the Microbiology Spectrum in 2022 that the combined use of nasal and throat swabs increased the positive percentage agreement to the real-time PCR by 88.7%. The value was just 64.5% with the samples from either site alone.

It means the virus doesn't clear equally from all body parts, and some organs continue to harbour it for a long time even though it has been cleared from other organs. The lymph nodes in the throat can clear the virus or its remnants much more rapidly, contributing to an earlier negative test.
Due to the uncertainty surrounding the tests, the scientific community has yet to reach a census. Taking the rapid test as a guide only and not a final authority has been recommended.
The development of the post-COVID condition
It is another condition which is worth mentioning. If you have recovered from the disease and tested negative but still have symptoms of the disease, you are likely to have the Post-COVID condition. It is also known as "long COVID" or post-acute sequelae of COVID-19 (PASC).
The potential factors responsible for the development of PASC are;
-
Acute injury to the multiple organs caused by the SARS-CoV-2
-
The development of a persistent reservoir of SARS-CoV-2 in any tissues
-
The interaction of the coronavirus with the normal microflora of the host
-
The reactivation of some other pathogens due to coronavirus infection
-
Autoimmunity due to the similarity of host and viral proteins
In this condition, you will continue to have the symptoms of COVID-19, e.g., fatigue, cognitive dysfunction, breadth short-sightedness etc. You can also get a positive result on a test. The other notable symptoms are chest pain, speaking difficulties, muscle aches, depression, anxiety, loss of smell and taste and fever.
Learn more about COVID-19 symptoms in our article Is tiredness a symptom of COVID-19?

How long this condition will linger? It needs to be clarified and completely understood. Some people have noted that these symptoms last for 3-6 months and potentially up to 9 months. However, more studies and follow up of the recovered patients are needed to understand it completely.
The treatment is often difficult and symptomatic. Besides the medication, the patients also need mental, psychological and social care. However, there is no specific treatment as there are a lot of ambiguities surrounding this condition.
You could have a false positive test.
The clinical diagnostic efficiency of a test is described in terms of sensitivity and specificity. The sensitivity of a test means its ability to correctly identify people with a disease. So, a low sensitivity means you are more likely to have a negative test while having a disease. Specificity is the ability of a test to correctly identify people without a disease. So, a low specificity means you may not have the disease but can have a positive test.
The antigen tests have less sensitivity (65.99%, as noted by a study published in the International Journal of Infectious Diseases in 2021) but good specificity (99.99%, noted by the same study.

Although the risk of false positive tests is slim, the risk is there.
COVID rebound, another cause of concern
It is the term used for the return of COVID symptoms after 2-8 days of recovery from primary infection. This issue is fairly common, as highlighted by a non-peer-reviewed study published in the medRxiv in 2022. The study involving 568 participants found that 12% of the patients had a viral rebound.
This phenomenon was for the first time observed in people who have received Paxlovid (explain); however, it can also be a normal part of disease progression in some people. Paxlovid is recommended to treat the symptoms of the early stage of the infection, particularly for people at a higher risk of developing hospitalisation and severe disease. The rebound can be a cause of concern, particularly if you are going to leave the isolation.

However, there is no evidence that the rebound of COVID can be as severe as the primary infection or the patient needs additional treatment. The patients experiencing the COVID rebound and continuing to have a positive antigen test are still infections and need 5 additional days of isolation to avoid spreading the virus to others.
Should you be worried if you have a positive test after 14 days?
The disappearance of clinical signs means that the body has cleared the virus. However, some viral antigens or their corresponding antibodies can still be present in the blood. Therefore, a positive test after the clinical signs have subsided is not a thing to be worried about. It doesn't necessarily mean that you are still infected. It means that the test is detecting the lingering viral antigens/ antibodies.
However, it would help if you continued to practice the safety precautions for more days.
Should you practice isolation if you are tested positive after 14 days?
According to the most recent WHO guidelines, a patient can end their isolation if the disease symptoms have improved and they hadn't developed a fever in the last 5 days. However, if the fever has subsided, but the respiratory systems haven't improved, a patient should continue to practice isolation or use control measures, e.g., a face mask for at least 10 more days.
A negative test is not the criteria to end isolation.
The current WHO guidelines don't require a person to be tested negative before ending the isolation. However, the people who choose to test can exit the isolation immediately if they are tested negative, while they should wait for 10 days if they are tested positive. The people with a negative test result should continue wearing masks for 10 more days after exiting the isolation.

It is still good to be on the safe side.
However, the international agencies have yet to develop any consensus on whether the patients should continue to isolate themselves for more days if they test positive. According to epidemiologists, people testing positive should continue to assume that they have an infection. It will allow them to be more careful about the people around them and will curb the spread of disease.
What would it mean to be immunocompromised?
Many problems experienced during an infectious disease are due to a poor immune system. Let's have some lines about this issue. An immunocompromised person is someone whose immune system is not working properly. A lot of factors and causative agents can lead to this issue, e.g.,
-
Anticancer chemotherapy or radiotherapy can kill the immune cells and cancer cells alike.
-
A recent organ transplant because the immune system is deliberately suppressed to avoid the risk of transplant rejection.
-
Use of immunosuppressant drugs, e.g., corticosteroids.
-
A recent stem cells transplant
-
The presence of any immunosuppression diseases, e.g., an advanced and untreated HIV
-
The use of anabolic steroids
What is the way forward?
Many people test positive even without any signs of disease for a long time. According to the experts, the safest way is to practice isolation until you receive a negative test result. If this is impossible, you can gradually leave the isolation even if you are still positive on a rapid test. It is particularly easy if you are fully vaccinated, and the symptoms have resolved.
However, you must practice other precautions, e.g., wearing a mask. In ideal situations, you should only stop using the mask once you get 2 negative tests 48 hours apart. Another alternative is to wear a mask for 10 additional days. If you suspect a mixing with others, use a high-quality mask, e.g., an N95 mask. In case of any complexity, seek the advice of an infectious disease specialist.
What is an FFP-2 mask? Learn more at Welzo.
Bottom-line
The emergence of coronavirus in 2019 was a shock to the medical community. Besides being a challenge for the medical community, it has also jeopardised the social and mental well-being of people throughout the globe. The initial recommendation was to end the isolation after the signs had subsided and the patient tested negative. But, the recommendations are continuously revised repeatedly according to discoveries and the appearance of new variants.

The disease caused by the original virus was acute and resolved rapidly as the viral load subsided. However, the emergence of new variants has changed the whole scenario. The new viruses are more adapted to the body than the original virus. A person can be tested positive even if the clinical signs have disappeared for up to 2 weeks.
It is also attributed to more sensitive tests that detect a few virus remnants. Although the consensus has yet to be achieved, it is recommended to isolate for 10 more days after you have tasted positive and continue to wear masks for 10 days after a negative test. In short, you should test negative before resuming your normal life.
At Welzo.com, our health professionals can guide you if you have prolonged COVID symptoms or are testing positive despite having no clinical signs. Our online pharmacy has treatments available for your symptoms. Click here to proceed.
For more information and guidelines, consult the local healthcare authorities.

















 Rated Excellent by 26,523+ Reviews
Rated Excellent by 26,523+ Reviews