What will the hospital do for sciatica pain?
.png?v=1669640216335)

Related products
What's covered?
What will the hospital do for sciatica pain?
The pain that radiates along the sciatic nerve's course is called sciatica. The sciatic nerve passes through the buttocks and hips before descending each leg from the lower back. The sciatic nerve is the body's thickest and largest nerve, measuring a finger's width. It directly affects how well you can move and feel your legs.

How are sciatic nerve and sciatica related?
The sciatic nerve comprises five nerve roots: three from the sacrum (the last segment of the spine) and two from the lumbar spine, located in the lower back. The right and left sciatic nerves form when the five nerve roots combine. One sciatic nerve per side of your body travels through the hip, buttock, and leg, ending just below the knee.
How does the sciatica pain feel?
Although true sciatic nerve damage is extremely rare, "sciatica" frequently describes pain originating from the lower back down the leg.
Depending on the reason, sciatica pain is described differently by various people. Some individuals report the pain as piercing, shooting, or jolting. Others call this pain scorching, electrical, or stabbing.
Additionally, compared to your lower back, your leg typically experiences more intense pain. Prolonged periods of sitting or standing, getting up, and twisting your upper body may worsen the pain. The sciatica pain can also get severe if you make a rapid, forceful movement like coughing or sneezing.
Sciatica affects one leg at a time. Sciatica can, however, manifest itself on both legs. It depends on where the nerve is being compressed along the spinal column.
What are the causes of sciatica pain?
Several conditions that affect your spine and the nerves that run along your back might lead to sciatica. The following are some common conditions that might result in sciatica,
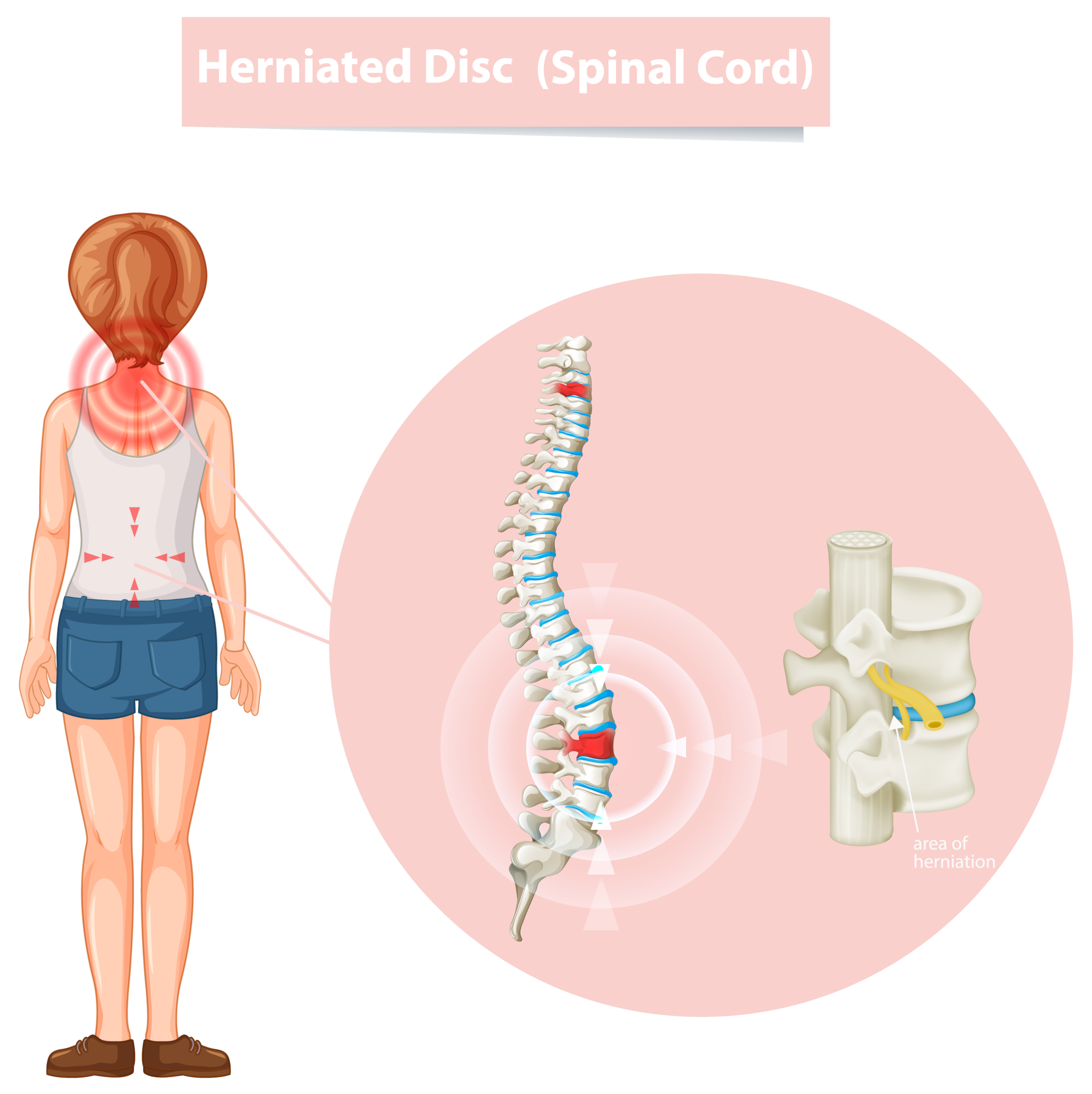
Herniated discs
Our bodies' vertebrae, or spinal bones, are divided by cartilage discs. Cartilage has dense, transparent material to maintain flexibility and cushion while moving around. When the surface layer of cartilage tears and herniated discs results. The sciatic nerve may become compressed by the internal material of the cartilage, causing a bulge or total spillage out of the disc, which would cause pain and numbness in your lower extremities. According to estimates, 1 to 5 per cent of all people will experience back pain brought on by a herniated disc at some time.
Piriformis syndrome
Piriformis syndrome is a disorder where the gluteal piriformis muscle spasms and causes buttock pain. This muscle attaches your thighbones to the lower part of your spine. The piriformis muscle may also irritate the neighbouring sciatic nerve, resulting in pain, tingling, and numbness in the foot and back of the leg (like sciatic pain).
Spondylolisthesis
One of the related conditions of degenerative disc disease is spondylolisthesis. The sciatic nerve may pinch off if one of the spinal bones or vertebrae stretches forward over another.
What is the treatment for Sciatica pain?
The main purpose of the treatment is to lessen the pain and increase mobility. Depending on the underlying cause, many sciatica patients improve gradually with a few straightforward self-care measures.
Non-surgical treatment options
Your doctor would first advise attempting some combination of these simple solutions if your pain is light and is not preventing you from going about your everyday business.
Physical therapy
Physical therapy aims to identify exercise techniques that lessen sciatica by relieving pressure on the nerve. Stretching activities should be included in an exercise routine to increase muscle flexibility, as should aerobic exercises (such as walking, swimming, and water aerobics). The doctor recommends a physical therapist who can work with you to create a stretching and aerobic exercise routine that suits your needs.
Stretching
Lower-back stretches can assist in reducing sciatica pain.
Exercises
Short walks can be a good option because inflammation can decrease when moving. Physiotherapists advise people with sciatica to do exercises that focus on the following:
-
Core toughness
-
Proper posture
-
Flexibility of hamstrings
-
Correct lifting methods
Your physical therapist can ensure that you are using the proper form to prevent future injury to yourself.
Hot and Cold Therapy
Therapy that alternates between hot and cold can speed up the healing process and reduce pain. The ice reduces inflammation, while the heat improves circulation as you alternate between heat and ice. While increased circulation promotes healing, decreased inflammation eases pain.
Cold therapy
Cold therapy can reduce inflammation as well as pain by
-
Cooling muscle fibres to reduce the frequency of muscle spasms
-
Causing blood vessels to constrict and blood flow to decrease, resulting in numbing sensations
-
Reducing skin's nerve conduction
Use ice packs as cold therapy for 15 to 20 minutes. If you continue to use ice, you risk developing frostbite, which could cause nerve damage.
Hot therapy
Heat therapy reduces sciatica pain. The benefits of heat therapy focus more on healing than on pain relief. Therefore, you should employ heat therapy after receiving pain relief from cold therapy. Heat therapy encourages recovery by:
-
Lowering spasms and tension in the muscles
-
Increasing joint flexibility
-
Enhancement of nerve tissue performance
-
The acceleration of tissue metabolism
You can use hot water bottles, hot packs, towels, or electric heating pads to administer heat therapy. To prevent skin injury, you should also avoid leaving hot pads on your skin for an extended period. For a discreet and consistent heat source, consider trying Cura-Heat warming patches.
Medications
Your doctor could suggest painkillers as the first line of treatment for sciatica. They can talk to you about restorative options once the discomfort has subsided. Patients who continue to experience pain following physical therapy sessions or other sciatic nerve treatments may additionally recommend painkillers. Medication for pain management is a temporary fix for severe discomfort. As a result, they are not practical as a long-term pain management strategy.
For sciatica pain, doctors frequently prescribe the following drugs
-
Non-steroidal anti-inflammatory drugs (NSAIDs)-Inflammation frequently occurs at the site where a disc or muscle is pressing on the sciatic nerve. NSAIDs reduce pain by preventing the body's inhibitors that cause inflammation. Find our range of NSAIDs here.
-
Opioid analgesics
-
Oral steroids
Epidural Steroid Injections
For many lower back and leg pain types, epidural steroid injections (ESIs) are a popular therapy option. They are a crucial component of the nonsurgical care of sciatica and lower back pain and have been utilized for decades.
The procedure is an epidural steroid injection because a local anaesthetic and steroid drug are injected directly into the epidural space, encircling the spinal cord and nerve roots.
Epidural Injection Approaches
This form of injection provides a steroid medicine with potent anti-inflammatory effects directly into the painful region close to the spinal nerve, which can result in quick and considerable pain relief. The doctors administer an epidural injection using any of the following methods:
-
Transforaminal route: This method enables accurate delivery of the steroid solution into the epidural space, close to the region where the nerve is most likely inflamed. This method of injection targets particular nerve roots to decrease pain and inflammation.
-
Interlaminar route: This procedure involves inserting the needle from the back of the spine. Because this technique does not place the drug close to the targeted nerve root and allows the steroid solution to move freely throughout the epidural region, it is less precise.
-
Caudal route: The drug does not directly target the cause of the pain in the epidural area, but it is easy to administer. Although the caudal technique is considered safer and simpler, it may be less successful. This technique might be useful for reducing generalized or scattered pain.
The benefits of epidural steroid injections are:
-
Reduce inflammation and nerve pain
-
Limit oral medication
-
Postpone surgery
Depending on their training, experience, guided fluoroscopy, and the outcomes of prior treatments for patients with similar illnesses, a doctor may decide which route of administration to take.
Specialists in treating pain and the spine, including physiatrists, anaesthesiologists, radiologists, neurologists, and spine surgeons, are some of the medical professionals who can administer this kind of injection. Typically, the injection procedure happens in a surgery centre, hospital, or doctor's office.
Nerve root block
A local anaesthetic and steroid (anti-inflammatory) solution is injected around a compressed or swollen spinal nerve during a nerve root injection. It is a highly popular procedure to help reduce nerve pain and inflammation.
The following medical benefit results from the use of local anaesthesia and corticosteroids together:
-
It stops the harmful inflammation process that causes pain and discomfort in the sciatic nerve.
-
They prevent specific nerve fibres from sending pain signals to the brain.
-
They reduce the blood flow to nerve fibres to lessen the transmission of pain.
-
Surgical options for sciatica
When leg pain persists or worsens, even after trying some non-surgical sciatica therapies, surgery for sciatica is typically considered. Surgery might be the first choice in a few situations.
Here are a few instances where having surgery is recommended as a first resort:
1. Cauda equina syndrome
Rarely, a herniated disc might irritate nerves to the point where you cannot control your bowels or bladder. The name of this condition is cauda equina syndrome. Left untreated, it can also result in paralysis, diminished sexual arousal, and tingling or numbness in the genital area. This condition frequently manifests slowly. You should visit your doctor or an emergency room immediately if the symptoms develop.
These are some signs of this disorder:
-
A lack of bladder or bowel control that may cause diarrhoea
-
Tingling or numbness in your legs
-
It is difficult to stand up after sitting due to weakness in one or both of your legs
-
Abrupt severe loss of feeling in the lower body, which includes the region between the legs, pelvis, inner thighs, heels, and entire foot, making it difficult to stand up.
2. Bilateral sciatica
It affects both legs and can be caused by disc herniation, acute single-level herniation, or spinal stenosis.
3. Spinal stenosis
Spinal stenosis is also known as lumbar spinal stenosis. The abnormal narrowing of the spinal canal is what gives it its name. This narrowing presses the sciatic nerve root and spinal cord, which results in sciatica pain.
Surgical Procedures
Microdiscectomy
Microdiscectomy is a surgical treatment of sciatica brought on by lumbar disc herniation. A small portion of the disc material beneath the nerve root and the bone covering the nerve root is removed during this operation. Although technically an open procedure, a microdiscectomy can be performed with only a small incision and little tissue damage by using minimally invasive procedures.
Lumber decompression surgeries
There are many surgical procedures available to treat several types of nerve root compression or irritation, including:
-
Laminectomy: In this treatment, the lamina is partially or completely removed to create greater spinal nerve space. It is typically performed for sciatica pain brought on by lumbar spinal stenosis. After lumbar laminectomy surgery, between 75% and 90% of patients may have pain alleviation.
-
Foraminotomy: The sciatic nerve root exits the spinal column through this opening, the neuroforamen, which is widened in this surgery by removing bony overgrowth.
-
Facetectomy: This surgical treatment reduces pressure on pinched nerves caused by degenerating facet joints. The facet joints are frequently clipped, undercut, or eliminated to reduce pressure on the nerves. According to estimates, 85% of individuals who have facetectomy surgery may feel pain reduction.
Risks of spinal surgery include infection, blood clotting, nerve injury, bowel movements and spinal fluid leak.
Sciatic Pain Diagnosis:
Your doctor or a spine specialist will investigate some issues about your discomfort and the signs and symptoms of sciatica. These inquiries might involve:
-
When did your discomfort begin?
-
What part of your body is in pain?
-
What causes your sciatica pain, specifically?
-
What is your usual level of activity?
-
What other symptoms do you experience besides pain?
-
How much do your symptoms and pain interfere with your everyday activities?

Following a physical and neurological examination, more tests may be performed based on your responses. The physical examination will assess the following:
-
Posture
-
Motion range
-
Overall state of health
-
Alignment and curvature of the spine
Your doctor will gently hold your legs and knees in various positions as part of the neurological exam to evaluate your reflexes, muscle power, and nerve function. The following are some examples of common sciatica diagnostic tests.
-
Computerized tomography scan (Ct scan)
-
X-ray
-
Medical resonance imaging (MRI)
-
Electromyography/Nerve Conduction Velocity test (EMG/NCV)
For targeted relief of back and leg discomfort, explore our back pain relief collection featuring topical treatments and supportive therapies.
Conclusion:
Most sciatica patients do not require surgery. Usually, all that is required is some time and self-care. However, visit a doctor if basic self-care measures fail to reduce your pain. Your doctor can identify the source of your discomfort, recommend alternative therapies, and, if necessary, send you to other spine health experts.
If you're looking for prescription, over-the-counter or drug-free pain relief, shop our products here.










 Rated Excellent by 26,523+ Reviews
Rated Excellent by 26,523+ Reviews