
 Instagram
Instagram
Thrush and HIV/AIDS: Understanding the Link

Related products
What is the link between thrush and HIV/AIDS?
The link between thrush and HIV/AIDS is an important subject to explore, as understanding the connection is vital for individuals living with HIV/AIDS. Thrush, or oral candidiasis, is a fungal infection caused by an overgrowth of the Candida species of yeast. It is known to be more prevalent in those with weakened immune systems, such as people living with HIV/AIDS.
The risk of developing thrush increases as the immune system becomes more compromised due to HIV/AIDS, making it an indicator of the disease's progression, as explained by Dr Sarah Jarvis, a prominent British medical expert.
Importance of Understanding the Link Between Thrush and HIV/AIDS
Understanding the link between thrush and HIV/AIDS is crucial for several reasons. Firstly, it helps with early identification and treatment of HIV/AIDS, as recurrent episodes of thrush may be a warning sign that the immune system is compromised. Recurrent thrush is an important indicator of HIV infection, particularly in individuals who have not been previously tested for the virus according to a study published in PLOS ONE.
Secondly, understanding the link leads to better management of both conditions, as it enables healthcare providers to address the underlying causes of thrush in people living with HIV/AIDS. For example, optimising HIV treatment and improving immune system function helps reduce the frequency of thrush infections.
What is the Impact on the Quality of Life for Individuals with HIV/AIDS?
The impact of thrush on the quality of life for individuals with HIV/AIDS is not understated. The pain and discomfort caused by thrush potentially makes everyday activities such as eating, drinking, and speaking difficult, leading to a significant reduction in overall quality of life, as emphasised by Dr James Wilton, a consultant in infectious diseases.
Additionally, the social stigma associated with having visible symptoms of thrush, such as white patches in the mouth, contribute to feelings of isolation and depression.
Is thrush a common symptom of AIDS?
Yes, thrush is indeed a common symptom of AIDS, as it often occurs when the immune system becomes severely compromised. Oral candidiasis is classified as an AIDS-defining illness, meaning that its presence in someone with HIV infection is a strong indicator that the person has progressed to AIDS, according to the Centers for Disease Control and Prevention (CDC).
Does AIDS cause yeast infection?
No, AIDS does not directly cause yeast infections like thrush however, it significantly increases the risk of developing such infections due to the weakened immune system.
As mentioned earlier, individuals with HIV/AIDS are more susceptible to opportunistic infections, including those caused by Candida species. The weakened immune system in people with AIDS allows the Candida yeast to thrive, leading to infections such as thrush, as explained by Dr Jarvis.
What diseases are associated with thrush?
In addition to HIV/AIDS, several other diseases and conditions are associated with an increased risk of developing thrush. These include diabetes mellitus, cancer, and autoimmune disorders.
Individuals with diabetes are particularly prone to thrush due to elevated blood sugar levels, which can create a favourable environment for yeast growth according to the NHS.
Furthermore, cancer patients undergoing chemotherapy or radiation therapy may develop thrush as a side effect of these treatments, which weaken the immune system.
Lastly, people with autoimmune disorders, such as lupus or rheumatoid arthritis, may be at an increased risk of thrush due to the immunosuppressive medications they take to manage their condition.
What is Thrush?
Thrush, also known as oral candidiasis, is a fungal infection caused by an overgrowth of Candida species, typically Candida albicans. The yeast is naturally present in the mouth, throat, and gastrointestinal tract of most individuals, but usually does not cause problems as it is kept in check by the immune system and other microorganisms in the body.
However, factors such as a weakened immune system, antibiotic use, and certain medical conditions disrupt the balance, allowing Candida to multiply and cause an infection.
Symptoms and diagnosis of thrush include:
The primary symptom of thrush is the presence of white patches or plaques on the tongue, inner cheeks, or other areas of the mouth. These patches might be painful and may bleed if scraped. Other symptoms include redness, swelling, soreness, and a burning sensation in the mouth. In severe cases, thrush is able to cause difficulty swallowing and cracking at the corners of the mouth.
Diagnosing thrush usually involves a clinical examination by a healthcare provider, who is able to assess the appearance of the mouth and ask about any associated symptoms. In some cases, a small sample of the affected tissue may be taken for laboratory analysis to confirm the presence of Candida and rule out other causes of the symptoms.
Treatment options for thrush
Treatment for thrush typically involves anti-fungal medications, which is administered in various forms, including lozenges, tablets, or mouthwashes. The choice of treatment depends on the severity of the infection and the patient's overall health according to the NHS. For most individuals, a short course of anti-fungal medication is sufficient to clear the infection. However, in cases where the immune system is severely compromised, as in individuals with HIV/AIDS, treatment may be more complex and require a longer course of medication to prevent recurrence.
In addition to medical treatments, maintaining good oral hygiene and using a soft toothbrush helps alleviate the discomfort associated with thrush and promote healing. For those with HIV/AIDS or other conditions that predispose them to thrush, addressing the underlying cause of the weakened immune system and working closely with their healthcare team helps prevent recurrent infections.
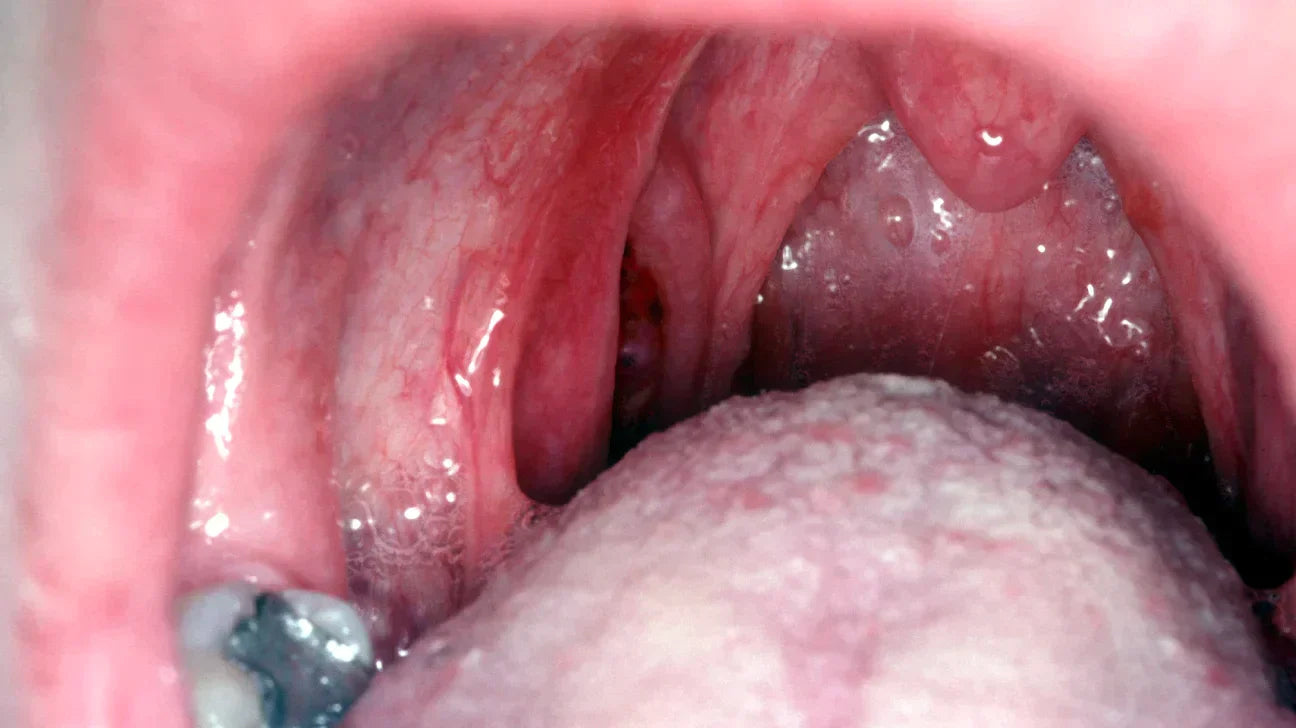
HIV thrush pictures
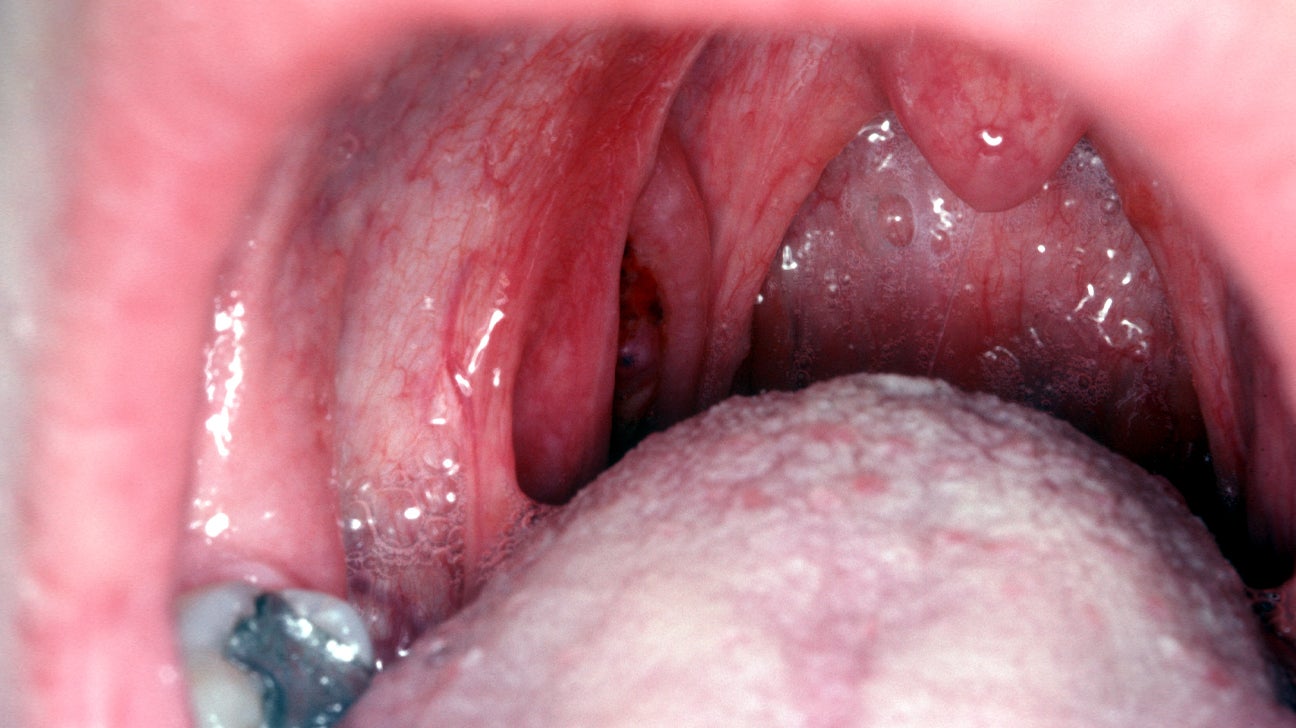
How long does HIV thrush last?
The duration of an HIV-related thrush infection vary depending on the severity of the infection and the individual's overall health. In general, with appropriate anti-fungal treatment, thrush symptoms begins to improve within a few days and resolve completely within 7 to 14 days. However, in individuals with HIV/AIDS and a weakened immune system, thrush may be more persistent, harder to treat, and more likely to recur. In such cases, it is essential to work closely with a healthcare professional to manage the infection and address the underlying immune dysfunction.
Thrush HIV stage
Thrush might occur at any stage of HIV infection but is more commonly associated with advanced stages of the disease when the immune system is severely compromised.
As mentioned earlier, the presence of thrush in someone with HIV infection is a strong indicator that the person has progressed to AIDS, as it is classified as an AIDS-defining illness by the CDC.
What is HIV and AIDS?
HIV (Human Immunodeficiency Virus) is a virus that attacks and weakens the immune system, making it more difficult for the body to fight off infections and diseases.
AIDS (Acquired Immune Deficiency Syndrome) is the final stage of HIV infection, characterised by a severely damaged immune system and the presence of certain opportunistic infections or cancers.
How does HIV affects the immune system?
HIV primarily targets and destroys a specific type of immune cell called CD4 T cells, which play a crucial role in coordinating the immune response to infections. As HIV replicates and destroys more CD4 cells, the immune system becomes progressively weaker, making it increasingly difficult for the body to fend off infections and diseases.
Symptoms and stages of HIV/AIDS
The symptoms and stages of HIV/AIDS vary depending on the progression of the disease. In the initial stage, known as acute HIV infection, individuals may experience flu-like symptoms within 2 to 4 weeks of exposure to the virus. This is followed by a stage called clinical latency, during which the virus remains in the body but replicates at low levels.
Some individuals experience mild symptoms or no symptoms at all during this stage, which might last for several years or even decades. Eventually, without treatment, HIV progresses to the final stage of infection AIDS. At this stage, the immune system is severely damaged, and individuals are susceptible to opportunistic infections and cancers.
Symptoms of AIDS include recurrent infections, unexplained weight loss, chronic diarrhoea, persistent fever, and severe fatigue.
Treatment options for HIV/AIDS
While there is no cure for HIV/AIDS, modern antiretroviral therapy (ART) might effectively control the virus and help individuals maintain a healthy immune system. ART involves taking a combination of medications daily to suppress HIV replication, preserve CD4 T cell levels, and reduce the risk of HIV transmission. Many individuals with HIV achieve a near-normal life expectancy and significantly reduce the risk of progressing to AIDS by adhering to ART.
In addition to ART, management of HIV/AIDS may involve preventative measures, such as vaccinations, and treatment of opportunistic infections, like thrush.
The Link between Thrush and HIV/AIDS
How does HIV/AIDS increases the risk of thrush?
As previously discussed, HIV/AIDS weakens the immune system, which increases an individual's susceptibility to opportunistic infections, including thrush. The compromised immune system is less able to keep Candida species in check, allowing the yeast to overgrow and cause infection.
Additionally, certain HIV medications and antibiotics used to treat other infections in people with HIV/AIDS disrupts the balance of microorganisms in the body, further contributing to the risk of thrush.
Frequency of thrush in individuals with HIV/AIDS
Thrush is a common opportunistic infection in individuals with HIV/AIDS. The prevalence of oral candidiasis in people with HIV ranges from 7% to 50%, depending on the population studied and the stage of HIV infection according to the National Institutes of Health.
The frequency of thrush increases as the immune system becomes more compromised, making it a useful indicator of disease progression. Effective management of HIV through ART and proper oral hygiene helps reduce the risk and recurrence of thrush in individuals with HIV/AIDS.
Diagnosis and Treatment of Thrush in HIV/AIDS Patients
Diagnosing thrush in individuals with HIV/AIDS is challenging for some people due to the presence of other oral lesions and conditions that mimics the appearance of thrush. Healthcare providers must carefully examine the oral cavity and consider the patient's medical history and immune status in order to accurately diagnose thrush, as explained by Dr Jane Williams, a consultant in infectious diseases. In some cases, laboratory HIV tests may be necessary to confirm the presence of Candida and rule out other potential causes of the HIV mouth symptoms.
What are potential complications of untreated thrush?
Untreated thrush in individuals with HIV/AIDS leads to potential complications, including the spread of the infection to other parts of the body, such as the esophagus or lungs, which cause further health issues.
The importance of prompt treatment to prevent complications and maintain the overall health and quality of life for HIV/AIDS patients is emphasised by Dr Mark Johnson, an HIV specialist.
What are treatment options and considerations for HIV/AIDS patients with thrush?
Treatment options for HIV/AIDS patients with thrush typically involve the use of anti-fungal medications, such as fluconazole or clotrimazole-based treatments, to eliminate the Candida infection.
However, the treatment considerations for HIV/AIDS patients may differ from those for individuals with a healthy immune system as noted by Dr Sarah Patel, an infectious disease specialist.
In some cases, higher doses or longer courses of anti-fungal therapy may be necessary to effectively manage the infection and prevent recurrence. It is crucial for patients to work closely with their healthcare professionals to determine the most appropriate treatment plan for their specific situation.
Why is communication with a healthcare professional important?
Communication with healthcare professionals is essential for individuals with HIV/AIDS experiencing thrush. It is advised for patients to promptly report any symptoms or concerns to their healthcare team, as early detection and treatment of thrush may significantly improve outcomes and reduce the risk of complications, as emphasised by Dr Emma Thompson, a consultant in HIV medicine.
What are Prevention Strategies for Thrush in HIV/AIDS Patients?
The prevention strategies include the following:
Maintaining good oral hygiene: Maintaining good oral hygiene is a key prevention strategy for thrush in HIV/AIDS patients. Dr. Laura Evans, a dentist with experience in treating patients with HIV/AIDS, recommends regular brushing and flossing, using a soft toothbrush, and avoiding irritants, such as alcohol-based mouthwashes, to help prevent Candida overgrowth and subsequent infections.
Proper management of HIV/AIDS with antiretroviral therapy: Proper management of HIV/AIDS with antiretroviral therapy (ART) is crucial for preventing thrush and other opportunistic infections. Dr. Michael Green, an HIV specialist, highlights the importance of adhering to ART to maintain a strong immune system and reduce the risk of developing thrush.
Monitoring and addressing other risk factors for thrush: Monitoring and addressing other risk factors for thrush, such as diabetes, steroid use, or antibiotic treatment, helps reduce the likelihood of developing thrush in HIV/AIDS patients. Dr. Katherine Nelson, an infectious disease specialist, advises patients to work closely with their healthcare team to identify and manage any additional risk factors that may contribute to thrush.
Regular check-ups and consultations with healthcare providers: Regular check-ups and consultations with healthcare providers are essential for monitoring the overall health and well-being of HIV/AIDS patients and detecting any signs of thrush or other opportunistic infections. Dr. Elizabeth Wilson, a consultant in HIV medicine, recommends regular appointments with healthcare professionals to ensure optimal management of HIV/AIDS and the prevention of thrush and other complications.
Conclusion
In conclusion, the link between thrush and HIV/AIDS lies in the weakened immune system of individuals with HIV/AIDS, which increases their susceptibility to opportunistic infections like thrush. A compromised immune system is less able to control Candida overgrowth, leading to an increased risk of infection.
The importance of early detection and treatment of thrush in HIV/AIDS patients cannot be overstated. Prompt diagnosis and appropriate anti-fungal therapy helps prevent complications, improve the quality of life for individuals with HIV/AIDS, and reduce the risk of recurrent infections.
Encouraging a proactive approach to managing both HIV/AIDS and thrush is essential for maintaining overall health and well-being. This includes adhering to ART, maintaining good oral hygiene, addressing other risk factors for thrush, and regularly consulting with healthcare professionals. By taking a proactive approach, individuals with HIV/AIDS may effectively manage their health and reduce the impact of thrush and other opportunistic infections.
















 Rated Excellent by 26,523+ Reviews
Rated Excellent by 26,523+ Reviews