Why Do I Keep Getting Thrush? Causes and How to Stop It
.png?v=1666084390547)

Related products

Thrush is a common yeast infection caused by a fungus called Candida albicans, affecting both men and women. It is usually harmless but can cause discomfort and is neither considered a bacterial nor a sexually transmitted infection. About 75% of women develop vaginal thrush at least once in their lifetime. Simple thrush infections are often easy to treat, and most women experience immediate relief from having medication.
However, despite adequate treatment, some women continue to get the infection (recurrent thrush). Thrush that stubbornly keeps on coming back can negatively impact a person's quality of life especially when it becomes difficult to determine where to start tackling these infections. In this post, possible causes of recurrent thrush are explored, along with available treatment options and tips for preventing repeated infections.
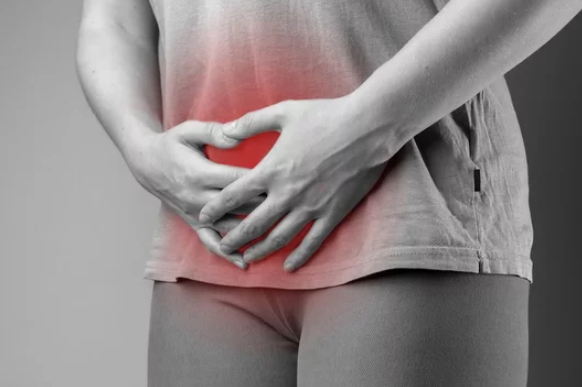
Vaginal thrush?
The vagina has natural defences such as mucus and healthy bacteria that protect it from excessive fungal growth. When these defences are disrupted by certain factors, fungi can enter and invade the vagina thereby causing the infection. Although it is not considered to be a sexually transmitted infection (STI), thrush can sometimes be caused by sex or transmitted between partners via intercourse. Also, vaginal thrush does not result from the lack of proper hygiene.
Often, no single cause of thrush is identified; but certain factors interfere with the vagina’s natural defences and increase the likelihood of developing the infection (and/or having recurring thrush). These factors include but are do not limit to:
-
Taking antibiotics
-
Exposure to oestrogen hormone - pregnant women, women of reproductive age, women who use hormone replacement therapy
-
Menopausal stage
-
Weakened immune systems - due to conditions such as HIV or medications such as chemotherapy or steroids
-
Poorly controlled diabetes
-
Damaged and/or inflammation of the skin around the vulva
-
Certain lifestyle choices - such as vaginal douching, frequently using panty liners, etc.
-
These factors may predispose you to develop thrush, but some women develop the infection (or experience recurrent thrush) without any apparent triggers. Experiencing any of these factors does not always mean a chance of suffering from recurrent thrush.
What is recurrent thrush?
Thrush is considered recurrent if four or more episodes of the infection happen to a person within a year. About 5 out of 100 women who develop the first episode of vaginal thrush eventually struggle with repeated episodes of thrush infection. They may find that new the same infections reappear after treatment or that the persistent symptoms that wax and wane are severely experienced despite the completion of treatment courses.
Symptoms of recurrent thrush
The symptoms of recurring thrush are similar to a regular thrush infection. Some women may notice that symptoms disappear completely between infections, while others suffer from ongoing symptoms that can progress or worsen at various times. These symptoms can be the following:
-
Itchy and irritated skin outside the vagina (vulva) and (or) inside the vagina
-
Vagina soreness
-
Unusual vaginal discharge that is non-smelling and appears creamy white and thick (often called “cottage cheese”)
-
Pain when urinating
-
Pain during sexual intercourse
Why do I have recurrent thrush?
For the most part, it is not uncomplicated why some women suffer from recurring bouts of thrush. Some women simply seem to be more prone to develop thrush infections than others, and several factors can contribute to thrush recurrence.
-
It is worth reiterating the importance of completing the entire duration of treatment in any given circumstance. Treatment for previous episodes of thrush that did not completely clear the infection either due to a too-weak or too-short treatment cycle or improper administering is one identified factor that leads to the recurrence of infection.
-
The thrush is caused by Candida fungus that is resistant to standard treatments. About two in 10 women are reported to have recurrent thrush that is caused by the strain C. glabrata, rather than the more common Candida albicans.
-
Reinfection of thrush through sexual intercourse (the infection is transmitted back and forth between partners).
-
Conditions or situations that entail a high risk of developing thrushes, such as diabetes and a weakened immune system
-
Hygiene products can also cause irritation that can lead to a thrush infection. Frequent cleaning of your vagina during a period can also flush out the good bacteria which are necessary to clean the genitals naturally.
-
Repetitive participation in activities that irritate the vulva, such as using douches, scented soaps, tight-fitting clothing, etc.
-
The symptoms are not caused by the recurrence of thrush but instead by other skin conditions and infections.
When should I see a doctor?
The indefinite and complex cause of thrush recurring is what makes immediate consultation with a health expert always advisable in case of suffering from repeated episodes of thrush. Long-term treatments, unlike what is available over the counter, may be necessary. Thrush is not a sexually transmitted disease, but a sexual health clinic is also able to evaluate, diagnose, and treat women suffering from recurrent bouts of the infection. The itchy sensation in the vulva is not always associated with thrush; it can be caused by many other conditions. Only a healthcare professional can safely and properly diagnose the condition.
Even when a history of successful treatment of thrush in the past, it is best to see a doctor if experiencing any of the following:
-
Any of the above-stated symptoms that may suggest you have a condition other than thrush
-
Are pregnant or trying to conceive
-
Under 16 or over 60 years of age
-
Have diabetes
-
Have a weakened immune system (attributed to chemotherapy or long-term steroid medication)
-
Have had a previous STI (or worried about being possibly exposed to an STI, e.g. via unprotected intercourse)
-
Symptoms do not subside after taking an over-the-counter thrush medication
-
Symptoms that are in some way different from those experienced in a previous episode of thrush
-
History of having a negative response to anti-thrush medications
What will happen when I see a doctor?
Consultation with a health professional aims to determine whether thrush is the actual cause of the symptoms experienced and to identify any factors that may make a person susceptible to the recurrence of the infection. If you suffer from a recurrence of thrush, your doctor may want to examine you and execute some tests such as the following:
- Vaginal swabs. This confirms the presence of thrush infection and identifies which species of Candida is the causative agent.
- A pH test. This checks the acidity level of your vagina and helps to distinguish between thrush and bacterial vaginosis (another condition that commonly causes abnormal vaginal discharge). This involves inserting a small test strip into the vagina. A change in colour on the test strip can confirm if thrush is likely the cause of the symptoms.
- Urine tests. This examines the presence of an infection, which can sometimes appear with similar symptoms to thrush. This test may also screen urine for sugar to check for diabetes, a condition that can result in recurrent thrush.
Treating recurrent thrush
Thrush is usually treated with a two-stage process. The first stage is for the doctor to prescribe anti-thrush medications to treat the ongoing infection. Known as the “induction course” of treatment, this usually involves either oral antifungals (Fluconazole) or intra-vaginal antifungals (Clotrimazole pessaries). A longer duration of treatment is likely to be recommended than has been taken for thrush infections in the past.
For the second stage of the process, two options are can be done, which are either having a course of treatment in case of the reappearance of the symptoms or completing a “maintenance course” of treatment which involves taking anti-thrush medication for about six months, aiming to significantly lower the amount of Candida present.
Both options are usually available with oral or intravaginal (pessaries) antifungals. The appropriateness of the treatment option and medication depends on individual circumstances, personal preferences, and past reactions to anti-thrush treatments.
Meanwhile, antifungal creams may also be prescribed to relieve vulvar symptoms (e. itching, soreness, and/or irritation) which are available in many pharmacies. A follow-up appointment is usually arranged at around 6 months, which can be done sooner should any concerns persist.
Does my partner require treatment for thrush?
In rare cases, thrush can be transmitted between partners during sexual intercourse. Treatment is unnecessary if your partner does not manifest any thrush symptoms. However, it is always best to see a doctor for an appropriate diagnosis should you or your partner be bothered about possible symptoms of thrush in men which include:
-
Irritation, itching, redness, swelling, and (or) a burning sensation around the head of the penis and (or)under the foreskin
-
Pain on pulling back the foreskin
-
Painful urination and (or) sex
-
White discharge from the penis
-
An unpleasant odour around the genital region
What if I'm pregnant or breastfeeding?
Developing thrush during pregnancy is not uncommon. Although it does not pose harm to the baby, it is important to seek advice from a doctor or midwife for anti-thrush treatment, rather than trying to treat it yourself. Treating thrush during pregnancy or while breastfeeding is quite different which is the intra-vaginal administration of anti-thrush medications (e.g. pessaries or creams) for both singular infections, and the “maintenance course” of treatment for recurrent episodes of thrush.
Can you keep using thrush medication, long-term?
Repeated use of thrush remedies to treat the recurrences is normally safe. A doctor must be consulted should the infection not go away after one treatment cycle. A thrush infection usually clears up within a week, but the antifungal treatment is recommended for up to 14 days. This duration should be entirely completed despite the disappearance of symptoms, as doing otherwise increases the chance of the infection coming back.
For recurring thrush, the treatment is usually taken for a longer period, possibly for up to six months. Long-term treatment with antifungal medication can cause the fungi to develop resistance against the treatment which the doctor will check for the patient.
Can you cure the infection completely?
Thrush infections may either resolve on their own or can be treated with antifungal drugs. These drugs help clear the Candida yeast which causes the infection. But, since Candida is a yeast that naturally lives on your skin, it can cause another infection in the future.
Avoiding the infection and its recurrence
The fungus that causes thrush thrives in warm, moist, airless environments. There are some general lifestyle and behavioural changes you can make to prevent the growth of this fungus. These lifestyle changes can help prevent a single episode of thrush and reduce the risk of infection recurring.
-
Saying no to too much food with high sugar contents
-
Avoiding tight-fitting clothes and underwear
-
Avoiding perfumed soaps and deodorants on the genitals, opting for water and emollients (moisturizers)
-
Avoiding sex until a current infection is treated
-
Changing the underwear right after exercise
-
Regularly changing sanitary pads and tampons during a period
-
Taking showers instead of baths
-
Fully completing any courses of thrush treatment
-
Reducing stress and having a healthy lifestyle
Conclusion
Recurrences of vaginal candidiasis usually do not cause long-term health problems in women. However, suffering from recurring episodes of thrush can hugely affect your mood, sexual relationships, and overall quality of life.
The most salient step in addressing the issue of recurring thrush is to have an appointment with a healthcare professional to help you identify any factors that may predispose you to the infection and further prescribe the most appropriate treatment regimen for you. Treatments become most successful upon strict compliance with the doctor’s advice and completion of the full course.
If you want to determine if you have thrush or any other urinary tract infections, start your online consultation by clicking here.
Should you continue to have recurring thrush despite proper medical care, you may be referred to a specialist gynaecology or genitourinary medicine (sexual health) clinic. Most women who experience recurrent thrush have at least some reduction in the frequency and/or severity of episodes after a carefully completed treatment.
Related Thrush and Fungal Treatments
- Buy Daktarin Cream
- Buy Daktarin Gel
- Buy Vagisil Creme
- Buy Canesten cream
- Buy Fluconazole
- Buy Canesten Combi Creme
- Buy Canesten Thrush Pack
- Buy Gyno-daktarin
- Buy clotrimazole
- Buy Canesten Thrush Duo
- Buy Diflucan
- Buy Scholl Fungal Treatment
- Buy Lamisil
- Buy Curanail
- Buy amorolfine
Thush Related Articles
- How to get rid of thrush quickly
- Immediate thrush relief
- Why do I keep getting thrush?
- How to treat thrush in women
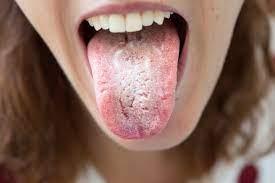
- Thrush on the tongue
- Thrush and diabetes
- Thrush and antibiotics
- Can stress cause thrush?
- Does thrush go away on its own?
- How to soothe thrush itching
- How long does it take to get rid of thrush?
- How to treat thrush in men?
- Thrush in babies
- Thrush and the elderly
- Is thrush an STI?
- Angular Cheilitis
- Vaginal thrush
- Thrush and HIV
- Best diet for candida
- Probiotics for thrush
- Thrush in animals
- Thrush and sexual health
- Thrush and the immune system
- Econazole
- Thrush pictures in females
- Nystatin for oral thrush
- Research advancements in thrush treatment
- Chronic yeast infections
- Can thrush cause bleeding?
- Esophageal thrush
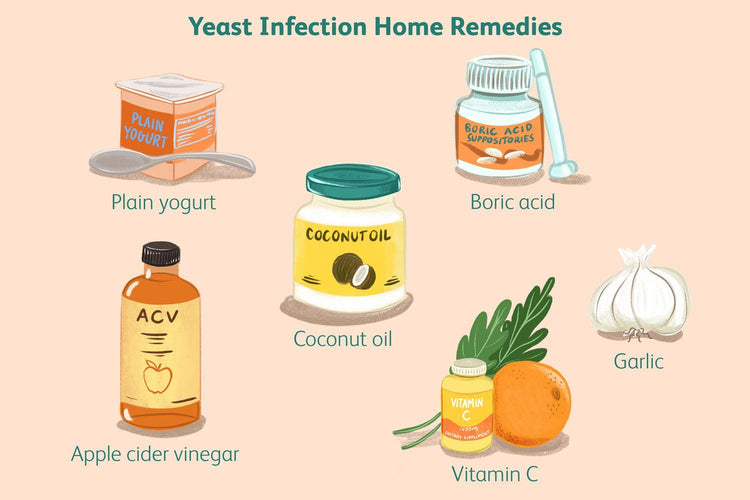
- Natural thrush remedies
- Breastfeeding thrush
- Nipple Thrush
- Is thrush contagious?
- Penile Thrush
- Recurring Thrush
- White Tongue: Causes, Treatments & Prevention
- Gentian Violet

































 Rated Excellent by 26,523+ Reviews
Rated Excellent by 26,523+ Reviews